health
Improving Lung Cancer Screening Compliance
Introduction
Lung cancer remains the leading cause of cancer-related deaths in the United States, claiming over 130,000 lives annually. Despite the availability of effective screening tools, the utilization of these services remains alarmingly low, with less than 1 in 5 eligible Americans up to date with lung cancer screenings. This article aims to delve into the reasons behind this low screening rate and explore strategies to improve compliance.
Benefits of Lung Cancer Screening
Lung cancer screening plays a pivotal role in reducing lung cancer mortality. By detecting lung cancer at an early stage, screening can increase the likelihood of successful treatment and improve overall survival rates. Low-dose computed tomography (LDCT) is the recommended screening method for individuals at high risk of developing lung cancer, including current or former smokers and those exposed to secondhand smoke.
Studies have consistently demonstrated the effectiveness of LDCT in reducing lung cancer mortality. The National Lung Screening Trial (NLST), a large-scale study involving more than 50,000 participants, found that annual LDCT screening reduced lung cancer-related deaths by 20% among high-risk individuals.
Barriers to Lung Cancer Screening
Despite the proven benefits of screening, several barriers contribute to the low compliance rate among eligible individuals. These include:
- Lack of Awareness: Many Americans are unaware of the importance of lung cancer screening and the criteria for eligibility. Misinformation and misconceptions about screening prevalent in the general population can further discourage individuals from seeking these services.
- Access to Care: Access to lung cancer screening can be limited in underserved communities and rural areas. Lack of insurance coverage and financial constraints can also pose barriers to screening.
- Fear and Anxiety: Some individuals may be hesitant to undergo screening due to fear of radiation exposure, discomfort, or a potential cancer diagnosis. Concerns about false positives and the potential for unnecessary follow-up procedures can also deter individuals from participating in screening programs.
- Physician Recommendations: The role of physicians in promoting lung cancer screening is crucial. However, some healthcare providers may not be adequately informed about the guidelines for screening or may not prioritize its discussion with patients.
Image by: https://www.news-medical.net/news/20220927/COVID-19-can-cause-long-term-lung-damage-to-children-and-teens.aspx
Improving Lung Cancer Screening Compliance
Addressing the barriers to lung cancer screening requires a multipronged approach involving healthcare providers, public health agencies, and the community. Key strategies to improve compliance include:
Increasing Awareness and Education:
- Public health campaigns should aim to increase awareness about lung cancer screening, its benefits, and the eligibility criteria.
- Healthcare providers should actively discuss screening with patients at risk and provide clear and accurate information about the procedure.
Expanding Access to Care:
- Expanding insurance coverage for lung cancer screening can improve access to these services for individuals who cannot afford the cost out-of-pocket.
- Establishing screening programs in community health centers and other underserved areas can make screening more accessible to vulnerable populations.
Reducing Fear and Anxiety:
- Providing accurate information about lung cancer screening can help alleviate fears and concerns.
- Emphasizing the potential benefits of early detection and the availability of low-dose radiation technology can help reduce anxiety.
- Offering emotional support and counseling services to individuals who are considering or have undergone screening can address the psychological aspects of the process.
Improving Physician Education and Recommendations:
- Continuing medical education programs and guidelines emphasizing lung cancer screening should be provided to healthcare providers.
- Incorporating screening reminders into electronic health records can help physicians identify eligible patients and initiate discussions about screening.
- Performance measures and incentives for lung cancer screening can encourage healthcare providers to prioritize this service.
Community Engagement and Outreach:
- Community-based initiatives, such as health fairs and educational events, can reach individuals who may not be aware of or actively seeking lung cancer screening.
- Partnerships with community organizations and advocacy groups can help promote screening and reduce stigma associated with lung cancer.
Conclusion
Addressing the low compliance rate of lung cancer screening is a critical public health challenge. By increasing awareness, expanding access to care, reducing fear and anxiety, improving physician education and recommendations, and engaging the community, we can empower more individuals to take advantage of this life-saving preventive measure. By ensuring that eligible Americans have access to and participate in lung cancer screenings, we can significantly reduce the burden of this devastating disease and save countless lives.
Beauty Fitness
Laser Hair Removal in Dubai: Advanced Technology

In the heart of Dubai, where luxury meets cutting-edge global innovation, every woman strives for a radiant look that reflects her self-confidence and natural beauty. One of the biggest challenges in daily personal care is the effective and permanent removal of unwanted hair. Fortunately, cosmetic solutions have evolved to become smarter and more comfortable, with laser hair removal in Dubai emerging as a leading option that combines medical precision with long-lasting, silky-smooth results.
The secret to lasting smoothness
Hair removal is no longer a routine procedure; it has become a relaxing and pampering experience. In Dubai, the latest laser technology, developed for 2026, is used, offering the ability to precisely target hair follicles without damaging the surrounding skin.
Why choose laser hair removal instead of waxing and shaving?
-
Long-lasting results: While waxing provides smoothness for only two weeks, laser gives you results that last for years after the sessions are completed.
-
Treating skin problems: Laser helps eliminate “chicken skin” and inflammation caused by ingrown hairs.
-
Lighter and smoother skin: The laser works to even out skin tone in areas that have darkened due to friction or traditional removal methods.
Laser technology
Beauty centers in Dubai pride themselves on offering advanced technologies suitable for all skin types and hair colors. Whether your skin is fair or dark, current technology guarantees safety and effectiveness.
Key technologies available:
-
Ice laser technology (Soprano): which provides continuous cooling to the skin, making the session completely painless and very suitable for sensitive areas.
-
The Candela Gentle Pro device: known for its powerful effectiveness in removing thick, fine hair with quick and precise touches.
-
Dual laser systems: which combine different types of light to safely suit dark and bronze skin tones.
How can you ensure you get the best results?
To get the most out of your laser hair removal experience in Dubai , an integrated approach should be followed, starting with pre-session preparation and ending with aftercare.
Expert tips for a perfect session:
-
Preparation beforehand: Make sure to shave the area with a razor 24 hours before your appointment, and avoid using any cosmetics or perfumes on the area.
-
Adherence to the schedule: Doctors recommend leaving a gap of 4 to 8 weeks between sessions to target hair in its active growth phase.
-
Continuous moisturizing: Use the soothing creams prescribed by your specialist to ensure your skin remains soft and supple after the session.
A smart investment of your time and money
Some might think laser hair removal is expensive, but when you look at the bigger picture, you’ll discover it’s an excellent investment. Think about how much you spend monthly on razors, hair removal creams, or regular salon visits. Laser hair removal saves you all that expense and effort, giving you lasting peace of mind and skin ready for any occasion, anytime.
Experience luxury in Dubai malls
What sets Dubai’s beauty services apart is not just the technology, but the luxurious environment in which the sessions take place. You’ll find professional medical teams, rooms equipped with the highest levels of sterilization, and customer service that guarantees your complete privacy and comfort. It’s not just a medical session; it’s a pampering beauty journey you deserve.
Common questions that might cross your mind:
-
Is laser treatment safe? Yes, it is a globally approved medical procedure and is completely safe when performed in licensed centers.
-
How many sessions do I need? The number usually ranges from 6 to 10 sessions to achieve near-complete hair removal.
-
Can laser hair removal be done in the summer? Absolutely, provided you use strong sunscreen and avoid direct tanning.
Pleased to share the rest of the article to cover the in-depth and detailed aspects that make this experience a complete beauty journey that goes beyond just hair removal:
Choosing the best technology according to your skin type
In Dubai, not all skin types are treated the same way, and this is the secret to the success of leading centers. Experts rely on the Fitzpatrick scale to determine the appropriate laser intensity and type for you, ensuring high effectiveness without any risks.
Alexandrite laser: For fair skin
If you have fair skin and dark hair, this device is the fastest and most efficient. It can cover large areas of the body (such as the legs and back) in record time, making it ideal for women with busy schedules.
Nd:YAG laser: for dark and tanned skin
Dubai is known for its cultural diversity, and therefore offers specialized technologies for darker skin tones. This type of laser operates at a longer wavelength, allowing it to penetrate the skin’s pigmentation and reach the hair follicle directly, making it the safest option for women with attractive darker skin tones, thus avoiding burns or pigmentation.
Laser hair removal for men in Dubai
Laser hair removal is no longer just for women; in recent years, beauty salons in Dubai have seen a surge in popularity among men. Whether the goal is precise beard shaping to eliminate folliculitis (razor bumps) or back and chest hair removal for a clean, athletic look, laser offers a practical, long-lasting solution that eliminates the hassle of daily shaving.
Factors that affect the success of sessions
To ensure your laser hair removal experience in Dubai is 100% successful, you should pay attention to some biological factors :
-
Hormonal equilibrium: Hormones are essential for hair development. In cases of disorders (like polycystic ovary syndrome), additional sessions or concurrent medical monitoring may be necessary to achieve sustainable outcomes.
-
Hair thickness and color: The darker and thicker the hair, the more it absorbs laser energy, resulting in faster results. However, modern technologies in 2026 are becoming more adept at treating fine, light-colored hair.
In short
Your path to perfect skin starts with a smart decision today. Getting rid of unwanted hair is no longer just a cosmetic issue. It’s part of your health and well-being, which reflects on your daily life. Dubai offers you all the resources to achieve this goal safely and luxuriously.
For a complete beauty experience that meets your aspirations, under the supervision of a select group of international experts, we invite you to visit the best beauty clinic in Dubai, where we promise you impressive results and outstanding service that guarantees you the lasting radiance and superior smoothness you deserve.
health
High Definition Liposculpture in Dubai: Body Sculpting Guide

When patients seek a sculpted, athletic appearance rather than simple fat reduction, High Definition Liposculpture in Dubai has become their procedure of choice. Unlike conventional liposuction, this technique is engineered to reveal the body’s natural muscle architecture — producing results that look earned, not operated upon. It sits at the intersection of surgical science and artistic precision, requiring a surgeon who understands anatomy at its deepest level.
What Exactly Is High Definition Liposculpture in Dubai?
High Definition Liposculpture in Dubai is an advanced fat removal and body contouring procedure that goes beyond standard liposuction. The goal is not merely to reduce fat volume but to sculpt and define the underlying musculature — including the abs, obliques, chest, arms, and flanks. Using ultrasound-assisted or laser-assisted energy, surgeons liquefy fat with surgical precision before removing it in layers that create dimension and shadow on the skin surface.
The procedure demands a nuanced understanding of superficial and deep fat compartments. Fat is selectively removed in specific zones to accentuate muscle edges, creating a three-dimensional contour that mimics natural athletic definition. In our clinical experience, the distinction between this and traditional lipo is immediately apparent during the consultation — patients are choosing a result, not just a reduction.
Technology Behind High Definition Liposculpture
Most HD Liposculpture procedures in Dubai are performed using VASER (Vibration Amplification of Sound Energy at Resonance) ultrasound technology. The VASER probe emits ultrasonic waves that selectively disrupt fat cell membranes while preserving surrounding nerves, blood vessels, and connective tissue. This selectivity is what makes true high-definition sculpting possible.
Once the fat is emulsified, it is removed with small cannulas in a precise, layered manner. The surgeon sculpts around the muscle anatomy rather than removing fat uniformly. The outcome is a surface of the body that clearly shows the underlying muscle groups.

Who Is the Right Candidate for This Procedure?
The ideal candidate is someone who is already at or near their healthy weight, maintains a relatively active lifestyle, and has good skin elasticity. Candidates often have persistent fat deposits that don’t respond to diet and exercise. Poor skin laxity or significant weight fluctuation history may affect result quality and requires careful evaluation.
In our clinical experience, the best outcomes occur in patients with realistic expectations who understand that HD Liposculpture enhances existing musculature — it does not create muscle that isn’t there. Patients should also be non-smokers, in good general health, and committed to maintaining their results through lifestyle choices.
Common Body Zones Treated
| Body Area | Muscles Highlighted | Typical Result |
| Abdomen | Rectus Abdominis, Obliques | Six-pack definition |
| Chest (Men) | Pectoralis Major | Defined chest contour |
| Arms | Biceps, Triceps | Lean, toned appearance |
| Flanks | Obliques, Love handle zone | V-taper silhouette |
| Thighs | Quadriceps, inner thigh | Elongated leg lines |
| Back | Trapezius, infrascapular | Defined upper back |
Step-by-Step: The Procedure Process
- Pre-operative consultation, 3D imaging, and surgical planning
- General or twilight anaesthesia administered
- Tumescent fluid injected to prepare the tissue
- VASER probe inserted to emulsify fat selectively
- Cannula removal of liquefied fat in precise layers
- Skin smoothed and compression garment applied
- Patient moved to recovery suite for monitoring
Recovery Timeline After High Definition Liposculpture in Dubai
| Phase | Timeline | What to Expect |
| Immediate | 0–72 hours | Swelling, soreness, compression garment required |
| Early Recovery | Week 1–2 | Reduced discomfort, light walking encouraged |
| Intermediate | Week 3–6 | Return to desk work, visible early contouring |
| Late Recovery | Month 2–4 | Progressive definition, most swelling resolved |
| Final Results | Month 4–6 | Full sculpted appearance visible |
Benefits That Make Patients Choose This Procedure
- Visible muscle definition rather than just fat reduction
- Long-lasting results when paired with a stable weight
- Minimal scarring due to small cannula entry points
- VASER technology reduces bleeding and shortens recovery
- Can be combined with fat transfer for augmentation
- Customisable to male or female aesthetic goals
Understanding the Cost Factors
Pricing for HD Liposculpture in Dubai varies depending on the number of zones treated, the technology used, surgeon expertise, and the facility. Treating multiple areas in a single session tends to be more cost-effective. A detailed quote is provided following your consultation and 3D imaging analysis.
Dubai-based providers are known for competitive pricing compared to Western markets, without compromising on quality, technology, or safety standards. Many clinics also offer flexible financing plans.
Side Effects and Safety Considerations
Common side effects include temporary swelling, bruising, numbness, and firmness in the treated area. These typically resolve within four to eight weeks. Serious complications are rare when the procedure is performed by a trained, board-certified surgeon in an accredited facility.
Patients are advised to disclose all medications, supplements, and medical conditions during their pre-operative assessment to minimise risk. Following post-procedure care instructions significantly reduces the chance of complications.
How to Maintain Your Results Long-Term
HD Liposculpture removes fat cells permanently from treated areas. However, remaining fat cells can still enlarge with significant weight gain. Maintaining a stable weight through balanced nutrition and regular exercise is essential to preserving your sculpted results.
What patients typically report during recovery is a growing motivation to maintain their physique — seeing early definition emerge becomes its own reward. Strength training and cardiovascular exercise support and enhance the visible definition achieved through the procedure.
Conclusion
If you are ready to move beyond standard body contouring and invest in precision sculpting that reflects your commitment to an active lifestyle, now is the time to act. Tajmeels Clinic offers high-definition body sculpting performed by specialist surgeons with deep anatomical expertise and a commitment to natural-looking results. Speak with our team to explore whether this transformative procedure aligns with your goals.
health
Paget Disease Treatment Market Growth, Trends & Forecast 2034

The United States holds a commanding share of the North American Paget disease treatment market. This dominant position stems from the nation’s highly advanced healthcare infrastructure. It also relies on high levels of disease awareness among clinicians. Furthermore, patients enjoy widespread access to specialized orthopedic and endocrinology care. A steadily expanding elderly population naturally supports this domestic market demand. This specific demographic faces a significantly higher susceptibility to chronic bone remodeling disorders.
On a global scale, the Paget disease treatment market is positioned for steady, predictable expansion. Financial projections indicate that the global market size will reach 2.96 billion dollars by the year 2034. This shows a clear increase from the 2.24 billion dollars recorded in 2025. This growth reflects a compound annual growth rate (CAGR) of 3.11% during the forecast period from 2026 to 2034.
Several primary catalysts fuel this upward trajectory. Rising international awareness of skeletal conditions leads the way. Significant advancements in diagnostic imaging technologies also accelerate growth. Additionally, a globally expanding geriatric population creates a larger patient pool. Finally, the widespread availability of highly effective pharmacological treatments keeps demand strong. Healthcare systems worldwide continue to prioritize better patient outcomes for chronic bone conditions. Consequently, the global demand for innovative therapeutic solutions expands every single year.
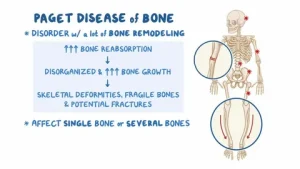
Key Drivers of Market Growth
Rising Prevalence of Chronic Bone Disorders
The growing prevalence of bone-related disorders among aging populations serves as a foundational driver for this market. Paget disease of bone is a chronic condition characterized by abnormal, accelerated bone remodeling. This disruption causes the body to produce enlarged, structurally weakened bones over time.
The disease remains relatively rare when compared to widespread conditions like osteoporosis or arthritis. However, its overall clinical incidence rises significantly as an individual ages. Global populations continue to grow older each year. Therefore, healthcare providers face an increasing number of patients who require medical diagnosis and long-term management for metabolic bone diseases. This mounting burden of musculoskeletal disorders prompts healthcare organizations to act. They are investing heavily in improved screening programs and public health awareness campaigns. Early detection allows for timely therapeutic intervention. This early care successfully reduces painful physical complications and supports long-term disease stability.
Advancements in Diagnostic Technologies
Technological breakthroughs in diagnostic imaging and laboratory testing play a vital role in fueling market expansion. Modern imaging modalities allow physicians to identify bone abnormalities much more accurately. These tools include high-resolution X-rays, nuclear bone scans, CT scans, and advanced MRI technologies. They help doctors catch the disease during its earliest, most manageable stages.
Beyond imaging, the market benefits from enhanced biochemical markers. Refined blood tests measure specific serum alkaline phosphatase levels. These tests provide clinicians with incredibly precise diagnostic data and reliable disease monitoring tools. These technical updates facilitate better overall treatment planning. They also help medical teams closely track how a patient responds to active therapy over time. As diagnostic accuracy improves across the globe, a larger percentage of patients receive appropriate care. This shift directly boosts the overall demand for prescriptions and clinical services.
Dominance of Bisphosphonate Therapies
Bisphosphonates remain the absolute cornerstone of modern Paget disease management. Consequently, this drug category represents the highest revenue-generating segment within the global marketplace. These specific medications work by regulating the body’s abnormal bone remodeling processes. They successfully slow down excessive bone resorption and reduce overall disease activity.
Several prominent drugs have demonstrated exceptionally strong clinical efficacy in controlling painful symptoms. These include zoledronic acid, alendronate, risedronate, and pamidronate. These medications consistently improve long-term patient outcomes. Extensive clinical evidence and favorable patient results strongly support the growing medical preference for bisphosphonate-based therapies. Patients also benefit from long-lasting disease control after completing their treatment regimens. Healthcare professionals routinely recommend these therapies as the primary, first-line treatment option. This established clinical habit will continue to drive substantial market revenue throughout the forecast period.
Emerging Opportunities in the Global Landscape
Growing Public Awareness and Early Diagnosis
Educational campaigns generate valuable new opportunities across the medical landscape. These initiatives are designed by healthcare organizations, patient advocacy groups, and government agencies. They work diligently to improve the general public’s understanding of rare bone conditions.
This growing awareness encourages individuals to seek professional medical evaluations much earlier. This is especially true for patients experiencing early warning signs like localized bone pain, skeletal deformities, or unexplained fractures. Early diagnosis does more than just improve immediate treatment outcomes. It actively minimizes the long-term risk of severe health complications, such as neurological compression or advanced joint arthritis. Educational initiatives continue to expand across both developed and emerging markets. Therefore, patient treatment adoption rates will scale up at a steady, predictable pace.
Expanding Healthcare Infrastructure in Emerging Markets
Emerging economies are quickly transforming into vital contributors to the global marketplace. Massive public and private investments are reshaping local healthcare infrastructures. These funding efforts expand patient access to specialized medical clinics. They also raise overall healthcare expenditures across developing regions.
These factors combined drastically improve diagnostic capabilities and treatment availability. This positive evolution is highly visible across the Asia-Pacific region, Latin America, and the Middle East. Local governments and private healthcare networks focus heavily on strengthening their medical delivery systems. They want to ensure that regional populations can obtain advanced therapies easily. These ongoing updates create excellent new growth pathways for international pharmaceutical manufacturers. They also open doors for healthcare providers specializing in bone management.
Research and Development Activities
Ongoing research initiatives aimed at uncovering the cellular mechanisms of Paget disease expand the market’s long-term potential. Pharmaceutical corporations and elite research institutions invest heavily in clinical studies. They want to explore innovative therapies, improved drug delivery formulations, and personalized medicine approaches.
These targeted methods could revolutionize daily disease management. Increased capital investments in clinical research are projected to yield a stronger pipeline of treatment innovations. As the scientific understanding of metabolic bone remodeling evolves, the market will benefit from next-generation therapeutic options. These future drugs will offer enhanced safety profiles and longer-lasting relief for patients.
The Competitive Landscape
The global Paget disease treatment marketplace features a highly competitive landscape. It is anchored by several prominent pharmaceutical giants. These corporations focus on developing, manufacturing, and commercializing advanced therapies for a wide range of bone disorders. To maintain their market positions, industry participants rely on a few core competitive strategies. These include forming strategic corporate collaborations, executing targeted product development initiatives, and pursuing rapid geographic expansion into untapped regions.
The leading players driving innovation and holding significant market share include:
-
Novartis AG
-
Pfizer Inc.
-
Merck & Co., Inc.
-
Teva Pharmaceutical Industries Ltd.
-
Amgen Inc.
-
Viatris Inc.
-
Sanofi SA
-
F. Hoffmann-La Roche Ltd.
-
Bayer AG
-
Sun Pharmaceutical Industries Ltd.
These industry leaders continue to funnel resources into their research and development wings. Their primary objective is to strengthen their existing product portfolios. By doing so, they can successfully address the shifting clinical needs of patients dealing with Paget disease.
Future Outlook
The global Paget disease treatment market is on track for steady, uninterrupted economic growth leading up to the year 2034. This upward trend relies on a combination of powerful demographic and technological factors. A growing global geriatric population provides a consistent foundation for treatment demand. Simultaneously, continuous advancements in diagnostic tools ensure that more patients find the care they need early on. The reliable clinical adoption of proven bisphosphonate therapies further cements this market security.
Healthcare systems across the globe are changing how they view chronic bone disorders. They now prioritize early medical intervention and structured, long-term patient care. Market participants are perfectly positioned to capitalize on these emerging global opportunities. Moving forward, a few critical factors will shape the true trajectory of this specialized market. Continuous product innovation will remain essential. Improving patient access to affordable healthcare services will also play a massive role. Finally, expanding clinician and patient education will ensure that high-quality care reaches every corner of the globe.
-
Business3 years ago
Cybersecurity Consulting Company SequelNet Provides Critical IT Support Services to Medical Billing Firm, Medical Optimum
-
Entertainment3 years ago
Meet the Megalodon: The Shark Star of ‘Meg 2’
-
Entertainment3 years ago
Reduce Video Game Lag: Level Up Your Gaming Performance
-
Sports3 years ago
Balancing India’s Entertainment: Cricket vs. Bollywood
-
Entertainment3 years ago
Jetsetter’s Secrets: Unveiling Our Favorite Travel Hacks for a Seamless Adventure
-
Productivity3 years ago
The 5 Best Live Sports Streaming Sites: Legal and Exciting!
-
Art /Entertainment3 years ago
Hollywood Labor Unrest: The Impact of ‘What About Us?’ Strikes
-
Sports3 years ago
Unveiling the Magic of Dream Fulfillment at the Late NBA Draft