health
Importance of Sleep: Maximizing Mental Clarity and Emotional Stability

Introduction
In our fast-paced world, the significance of sleep often gets overlooked. However, sleep plays a crucial role in our mental and emotional well-being. Understanding its importance is vital for maintaining a healthy lifestyle.
Define the Importance of Sleep
Sleep is a natural, recurring state of rest for the body and mind, characterized by altered consciousness, reduced sensory activity, and inactivity of nearly all voluntary muscles. It is essential for overall health and functioning.

Image by; yandex.com
Explain Its Relevance and Importance
Quality sleep is linked to improved cognitive function, emotional regulation, and physical health. It allows the body to repair tissues, consolidate memories, and regulate hormones. Lack of sleep can lead to a range of issues, including impaired judgment, mood disturbances, and increased risk of chronic diseases.
Types and Categories
Understanding the different types and categories of sleep can provide insights into its importance and impact on health.
Stages of Sleep
- Stage 1 (NREM): Transitioning from wakefulness to sleep, characterized by slowed eye movements and relaxed muscles.
- Stage 2 (NREM): Deeper sleep where brain waves slow down, and body temperature decreases.
- Stages 3 and 4 (NREM): Deep sleep stages crucial for physical restoration and growth.
- REM (Rapid Eye Movement) Sleep: Dreaming occurs, and brain activity increases, promoting cognitive function.
Sleep Disorders
- Insomnia: Difficulty falling or staying asleep, often resulting in fatigue and irritability.
- Sleep Apnea: Breathing pauses during sleep, leading to poor sleep quality and increased risk of cardiovascular problems.
- Narcolepsy: Excessive daytime sleepiness and sudden loss of muscle control, impacting daily activities.
- Restless Legs Syndrome (RLS): Uncomfortable sensations in the legs, causing an irresistible urge to move them, disrupting sleep.
Symptoms and Signs
Recognizing the signs of sleep deprivation or sleep disorders is crucial for addressing underlying issues.
Common Symptoms of Sleep Deprivation
- Daytime Fatigue: Feeling tired despite adequate time spent in bed.
- Mood Changes: Increased irritability, mood swings, or feelings of depression.
- Poor Concentration: Difficulty focusing on tasks or making decisions.
- Memory Problems: Forgetfulness and difficulty retaining information.
- Physical Symptoms: Headaches, muscle aches, and gastrointestinal issues.
Signs of Sleep Disorders
- Loud Snoring: A common symptom of sleep apnea.
- Gasping or Choking: Waking abruptly with a sensation of suffocation.
- Excessive Daytime Sleepiness: Feeling drowsy or falling asleep during activities.
- Leg Twitching: Involuntary leg movements during sleep, indicative of RLS.
- Sleepwalking or Nightmares: Unusual behaviors during sleep, indicating potential sleep disorders.
Causes and Risk Factors
Understanding the underlying causes and risk factors can help prevent sleep disturbances and promote better sleep hygiene.
Biological Factors
- Brain Activity: Disruptions in neurotransmitters or brain waves can affect sleep patterns.
- Genetics: Certain genetic factors may predispose individuals to sleep disorders.
- Hormonal Changes: Fluctuations in hormones, such as melatonin and cortisol, influence sleep-wake cycles.
Environmental Factors
- Noise and Light Pollution: External stimuli can disrupt sleep and affect its quality.
- Temperature: Extreme temperatures or uncomfortable sleep environments impact sleep comfort.
Lifestyle Factors
- Stress and Anxiety: Mental health conditions contribute to sleep disturbances.
- Poor Sleep Habits: Irregular sleep schedules or excessive screen time before bed disrupt sleep patterns.
- Diet and Exercise: Consuming stimulants like caffeine or lack of physical activity can affect sleep quality.
Diagnosis and Tests
Proper diagnosis is essential for identifying sleep disorders and developing effective treatment plans.
Medical Evaluation
- Clinical Assessment: Detailed history-taking and physical examination by a healthcare provider.
- Sleep Diary: Recording sleep patterns, habits, and symptoms over time.
- Polysomnography: Overnight sleep study monitoring various physiological parameters.
- Multiple Sleep Latency Test (MSLT): Assessing daytime sleepiness and detecting narcolepsy.
Home Sleep Tests
- Portable Monitoring Devices: Non-invasive tools for diagnosing sleep apnea in the home setting.
- Actigraphy: Using wrist-worn devices to track movement and sleep-wake cycles.
Treatment Options
Effective treatment strategies aim to improve sleep quality and address underlying sleep disorders.
Medical Treatments
- Continuous Positive Airway Pressure (CPAP): Gold standard treatment for obstructive sleep apnea.
- Medications: Prescription drugs for insomnia, narcolepsy, or RLS symptoms.
- Surgical Interventions: Procedures to alleviate sleep apnea or correct anatomical abnormalities.
Therapies and Interventions
- Cognitive Behavioral Therapy for Insomnia (CBT-I): Behavioral techniques to modify sleep habits and improve sleep quality.
- Relaxation Techniques: Yoga, meditation, or progressive muscle relaxation to reduce stress and promote relaxation.
Preventive Measures
Incorporating healthy sleep habits and lifestyle modifications can prevent sleep disturbances and promote restful sleep.
Sleep Hygiene Tips
- Consistent Sleep Schedule: Establishing a regular sleep-wake cycle to regulate circadian rhythms.
- Optimal Sleep Environment: Creating a comfortable and conducive sleep environment free from disruptions.
- Limiting Stimulants: Avoiding caffeine, nicotine, and alcohol close to bedtime.
- Screen Time Management: Minimizing exposure to electronic devices before bedtime to promote relaxation.
- Mindfulness Practices: Practicing relaxation techniques or mindfulness meditation to reduce stress and promote sleep.

Image by: yandex.com
Personal Stories or Case Studies
Real-life experiences provide valuable insights into the impact of sleep on individuals’ lives.
Case Study: Overcoming Insomnia
Sarah, a busy professional, struggled with chronic insomnia for years. Despite trying various remedies, she found relief through cognitive behavioral therapy. By addressing underlying stressors and adopting healthy sleep habits, Sarah regained control over her sleep and improved her overall well-being.
Expert Insights
Medical professionals offer valuable perspectives on the importance of sleep and strategies for optimizing sleep health.
Dr. Emily Johnson, Sleep Specialist
“Quality sleep is essential for physical and mental health. By prioritizing sleep hygiene and seeking timely evaluation for sleep disturbances, individuals can optimize their sleep health and improve their quality of life.”
Conclusion
Sleep plays a vital role in maintaining mental clarity and emotional stability. By understanding its importance, recognizing sleep disorders, and adopting healthy sleep habits, individuals can enhance their overall well-being and quality of life.
health
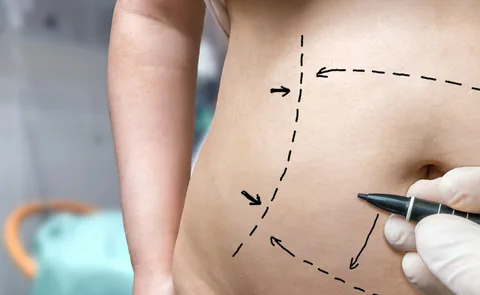
Mini vs Full Tummy Tuck: Complete Guide Islamabad
Beauty Fitness
Liposuction: Cheap vs Premium Clinics for Effective Results

Liposuction in Islamabad is becoming increasingly popular among people looking to achieve a slimmer body. With many clinics offering varying prices, it’s essential to understand the difference between cheap and premium options. Your choice can affect both the results and your safety.
Understanding Cheap Liposuction in Islamabad
Cheap Liposuction in Islamabad is often chosen by patients looking for affordable ways to remove stubborn fat. The lower cost can make the procedure appealing, especially for those on a tight budget. However, it’s important to understand what “cheap” really means in this context. Often, these procedures may use older equipment or be performed in clinics with less experienced staff.
While cheap Liposuction in Islamabad can deliver results, the quality of care and safety may not match premium clinics. There is a higher chance of complications such as uneven fat removal, infection, or longer recovery periods. Patients should carefully research the clinic, check surgeon qualifications, and read patient reviews before deciding.
Natural ways to prepare for surgery, such as maintaining a balanced diet and regular exercise, can improve outcomes regardless of the clinic you choose. Aftercare is equally important, but some budget clinics may not provide comprehensive guidance.
In short, cheap Liposuction in Islamabad can be an option for those mindful of costs, but safety and results should remain a priority. Investing time in research and preparation ensures you achieve better outcomes while minimizing risks.
Premium Liposuction in Islamabad
Premium Liposuction in Islamabad offers advanced technology and highly trained surgeons. Clinics offering premium services provide a safer environment and personalized care. The procedure usually results in smoother outcomes and faster recovery. While more expensive, the long-term benefits are often worth the investment.
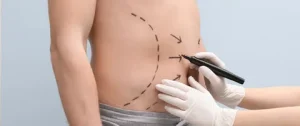
Key Differences Between Cheap and Premium Liposuction
Here are some major points to consider when choosing between cheap and premium Liposuction in Islamabad:
- Cost vs Safety: Cheap options save money but may compromise on safety.
- Experience of Surgeons: Premium clinics employ certified, experienced professionals.
- Equipment Quality: Advanced tools in premium clinics ensure better results.
- Aftercare Support: Premium clinics provide structured follow-up for recovery.
- Hospital Standards: Higher-end clinics follow strict hygiene and safety standards.
Why Cost Shouldn’t Be the Only Factor
While affordable Liposuction in Islamabad is tempting, focusing solely on cost can be risky. Quality of care, surgeon expertise, and clinic standards directly impact your results. Natural ways to prepare for surgery, like maintaining a healthy diet and exercise routine, can improve outcomes regardless of the clinic you choose.
Recovery and Aftercare
Recovery and aftercare are crucial steps following Liposuction in Islamabad to ensure safe healing and optimal results. After the procedure, patients may experience swelling, bruising, or mild discomfort. These are normal and usually subside within a few weeks. Following your surgeon’s instructions is essential to minimize complications and achieve the desired outcome.
Most premium clinics recommend wearing compression garments to support the treated areas. These garments help reduce swelling and contour the body shape. Pain management is also important, and your doctor may prescribe mild medications to ease discomfort. Regular check-ups during the first few weeks allow the surgeon to monitor healing progress.
Incorporating natural ways to enhance recovery can be very effective. Eating a balanced diet, staying hydrated, and engaging in light physical activity, such as short walks, can boost circulation and aid in faster healing. Avoiding smoking and alcohol is highly recommended as they can slow down the recovery process.
Proper aftercare also involves maintaining hygiene around the incision sites and promptly reporting any unusual symptoms to your surgeon. Choosing a reputable clinic ensures structured guidance, making your Liposuction in Islamabad experience safer and more satisfying.
Choosing the Right Clinic
Selecting the right clinic for Liposuction in Islamabad requires research. Look for reviews, surgeon credentials, and patient testimonials. Visiting the clinic before surgery helps you understand the environment and professionalism. Investing in a reputable clinic ensures your safety and satisfaction with the results.
FAQs About Liposuction in Islamabad
Q1: Is cheap liposuction safe?
A1: While possible, cheap Liposuction in Islamabad often carries higher risks due to older equipment or less experienced surgeons.
Q2: How long is the recovery time?
A2: Recovery usually takes 2–4 weeks, but premium clinics provide better guidance to speed up healing.
Q3: Can natural ways improve liposuction results?
A3: Yes, healthy diet, light exercise, and hydration help enhance results and reduce complications.
Q4: How do I choose between cheap and premium options?
A4: Evaluate clinic reputation, surgeon experience, equipment quality, and aftercare before deciding.
Q5: Are the results permanent?
A5: Liposuction in Islamabad provides long-lasting results if a stable lifestyle and natural ways of maintaining weight are followed.
Final Thoughts
Choosing between cheap and premium Liposuction in Islamabad is about balancing cost and safety. Prioritizing quality ensures better results, faster recovery, and minimal risk. For those seeking the best care and outcomes, trusted clinics like skn cosmetics offer professional services that meet international standards.
Care
Top Reasons Adults Choose Hormone Replacement Services in Houston
Hormone changes are a normal part of aging. As you get older, your body may not produce hormones at the same levels as before. These shifts can affect how you feel day-to-day, including your energy, sleep, mood, and focus. Many adults living in Houston begin to notice these changes and look for ways to better understand what is happening in their bodies.
Some people try to adjust their lifestyle first. They may improve their diet, exercise more, or work on sleep habits. While these steps are helpful, they do not always address hormone-related concerns fully. This is where structured evaluation and care can help.
Hormone-focused services look at your symptoms and lab test results to understand your body more fully. Instead of guessing, you receive information based on measurable data. This helps guide decisions and next steps in a clearer and more practical manner.
Key Reasons Adults Turn to Hormone Replacement in Houston Care
-
Addressing low energy that affects daily life
Many adults feel tired even after enough sleep, which can affect daily tasks and focus. Hormones such as thyroid hormone and testosterone help regulate energy levels. When these hormones are out of balance, you may feel drained without a clear reason.
Testing helps determine whether hormones are the cause, and care plans can then include hormone support, along with routine and nutrition guidance, to address the root issue rather than just the symptoms.
-
Supporting mood changes and mental clarity
Hormones influence brain function, including mood and concentration. When levels shift, you may notice irritability, stress, or difficulty staying focused.
These changes can affect your relationships, work, and overall quality of life. By reviewing hormone levels, a provider can look for patterns that may explain these symptoms. In some cases, adjusting hormone levels may help support more stable mood and clearer thinking.
This process is often combined with lifestyle habits such as regular sleep, balanced meals, and stress management techniques.
-
Managing natural hormone decline with age
Hormone levels change as part of the aging process. This happens in both men and women, although the patterns may differ.
For example, testosterone levels may decrease in men over time, while women may experience changes in estrogen and progesterone. These shifts can bring noticeable symptoms that develop slowly.
Regular evaluation helps track these changes over time. With ongoing monitoring, you and your provider can make informed decisions about whether support is needed and how to adjust care as your body changes.
-
Improving sleep quality and patterns
Sleep issues are often linked to hormone imbalance. Hormones such as cortisol and melatonin help regulate your sleep cycle.
If these hormones are out of balance, you may find it hard to fall asleep or stay asleep through the night. Poor sleep can then affect energy, mood, and overall health.
In cases where sleep problems are linked to hormones, evaluation can help identify the cause. Care may include hormone-related support, along with habits such as maintaining a consistent sleep schedule, limiting screen time before bed, and creating a calm sleep environment.
-
Supporting weight management efforts
Weight changes can be influenced by hormone levels. Hormones help regulate metabolism, appetite, and fat storage.
Some adults follow diet and exercise routines but still find it difficult to manage their weight. In these situations, hormone testing may provide more insight into what is happening inside the body.
A provider may review hormones related to metabolism, such as thyroid hormones and insulin. Based on the results, a plan may include a mix of hormone support, nutrition guidance, and physical activity recommendations.
-
Improving physical performance and recovery
Hormones also play a role in muscle strength, endurance, and recovery after exercise.
If your hormone levels are not balanced, you may notice reduced performance during workouts or longer recovery times. This can make it harder to stay consistent with fitness routines.
By checking hormone levels, providers can identify areas that may be affecting your physical performance. With proper guidance, you may see improvements in strength, stamina, and recovery when combined with regular exercise and proper rest.
-
Personalized care with ongoing monitoring
One main reason adults choose hormone-related services is the structured, personalized approach. Care is not a one-time visit. It usually includes consultation, lab testing, a tailored plan, follow-ups, and adjustments based on progress.
This step-by-step process helps track changes over time and ensures care is updated based on how your body responds. When considering options like hormone replacement in Houston, many adults prefer services that combine testing, guidance, and ongoing support for a clearer path forward.
Summary!
Hormone-related concerns can affect many areas of daily life, including energy, sleep, mood, weight, and physical performance. As these changes develop over time, it can be helpful to look at your health in a structured way that includes both testing and ongoing evaluation.
Choosing hormone-focused care allows you to better understand what is happening inside your body and take informed steps based on real data. With the right approach, you can work toward better balance while maintaining your daily routine and lifestyle.
In Houston, PUUR Health and Wellness offers a care model that focuses on personalized evaluation, monitoring, and guided support. This type of approach helps you move forward with clarity and consistent follow-up as part of your overall wellness plan.
-
Business3 years ago
Cybersecurity Consulting Company SequelNet Provides Critical IT Support Services to Medical Billing Firm, Medical Optimum
-
Business3 years ago
Team Communication Software Transforms Operations at Finance Innovate
-
Business3 years ago
Project Management Tool Transforms Long Island Business
-
Business3 years ago
How Alleviate Poverty Utilized IPPBX’s All-in-One Solution to Transform Lives in New York City
-
health3 years ago
Breast Cancer: The Imperative Role of Mammograms in Screening and Early Detection
-
Sports3 years ago
Unstoppable Collaboration: D.C.’s Citi Open and Silicon Valley Classic Unite to Propel Women’s Tennis to New Heights
-
Art /Entertainment3 years ago
Embracing Renewal: Sizdabedar Celebrations Unite Iranians in New York’s Eisenhower Park
-
Finance3 years ago
The Benefits of Starting a Side Hustle for Financial Freedom