health
How Telemedicine is Improving Access to Specialty Care

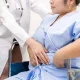
In recent years, telemedicine has revolutionized the healthcare landscape, offering unprecedented access to medical services through the use of digital technology. One of the most significant impacts of telemedicine has been its ability to improve access to specialty care, addressing both geographical and logistical barriers that have traditionally limited patient access to specialized medical expertise. This article explores how telemedicine is transforming specialty care, the benefits it brings to patients and healthcare providers, and the challenges that still need to be addressed.
The Role of Telemedicine in Specialty Care
Telemedicine refers to the use of telecommunications technology to provide clinical health care from a distance. It encompasses a broad range of services, from video consultations and remote monitoring to digital transmission of diagnostic images and patient data. Telemedicine Specialty Care specifically involves the provision of specialized medical services, such as cardiology, neurology, dermatology, and psychiatry, through these digital platforms.
Bridging Geographical Gaps
One of the primary advantages of telemedicine in specialty care is its ability to bridge geographical gaps. Patients living in rural or underserved areas often face significant challenges in accessing specialist care. These regions may lack the necessary medical infrastructure or have a limited number of specialists, forcing patients to travel long distances for consultations and treatments.
Telemedicine eliminates the need for physical travel, allowing patients to connect with specialists from the comfort of their homes. This is particularly beneficial for individuals with mobility issues, chronic illnesses, or those who require frequent follow-ups. By leveraging telemedicine, healthcare providers can extend their reach to remote areas, ensuring that patients receive timely and appropriate care regardless of their location.
Reducing Wait Times
In many regions, the demand for specialty care far exceeds the available supply of specialists, leading to long wait times for appointments. This delay can be detrimental to patients with serious or progressive conditions, as timely intervention is often crucial for effective treatment.
Telemedicine can significantly reduce wait times by streamlining the consultation process. Virtual appointments can be scheduled more flexibly, and specialists can manage their time more efficiently, seeing more patients in a shorter period. Additionally, telemedicine platforms often include features like electronic medical records and automated appointment reminders, which further enhance the efficiency of the care delivery process.
Enhancing Continuity of Care
Continuity of care is a critical aspect of effective healthcare, particularly for patients with chronic conditions that require ongoing management. Telemedicine facilitates continuous monitoring and follow-up, enabling specialists to track patients’ progress and make necessary adjustments to their treatment plans.
For example, a cardiologist can remotely monitor a patient’s heart rate and blood pressure using wearable devices, while a dermatologist can review high-resolution images of a patient’s skin condition. These capabilities allow for more proactive and personalized care, reducing the risk of complications and improving overall health outcomes.
Expanding Access to Expertise
Telemedicine also democratizes access to specialized medical expertise. In traditional healthcare settings, patients are often limited to the specialists available within their local healthcare network. Telemedicine breaks down these barriers, allowing patients to consult with top specialists from across the country or even internationally.
This expanded access to expertise is particularly valuable for rare or complex conditions that require highly specialized knowledge. Patients can seek second opinions, access cutting-edge treatments, and benefit from the latest advancements in medical research, all through virtual consultations.

Picture by: Yandex.com
Benefits for Healthcare Providers
The advantages of telemedicine in specialty care extend beyond patients to healthcare providers as well. By adopting telemedicine, specialists can optimize their practice, improve patient satisfaction, and enhance their professional development.
Increased Efficiency and Productivity
Telemedicine allows specialists to manage their time more effectively, reducing the downtime associated with in-person appointments. Virtual consultations can be scheduled back-to-back, minimizing the gaps between appointments and maximizing the number of patients seen in a day.
Moreover, telemedicine platforms often integrate with electronic health records (EHR) systems, streamlining administrative tasks such as documentation, billing, and prescription management. This integration reduces the administrative burden on healthcare providers, allowing them to focus more on patient care.
Professional Collaboration and Knowledge Sharing
Telemedicine fosters collaboration and knowledge sharing among healthcare providers. Specialists can easily consult with their peers, participate in virtual case discussions, and access a wealth of online resources and training materials. This collaborative environment promotes continuous learning and professional development, ultimately enhancing the quality of care provided to patients.
Financial Benefits
Adopting telemedicine can also have financial benefits for healthcare providers. By expanding their reach to a broader patient base, specialists can increase their revenue streams. Additionally, telemedicine can reduce overhead costs associated with maintaining physical office spaces and administrative staff.
Challenges and Considerations
While telemedicine offers numerous benefits, there are also challenges and considerations that need to be addressed to fully realize its potential in specialty care.
Technology and Infrastructure
The successful implementation of telemedicine relies on robust technology and infrastructure. This includes reliable internet connectivity, secure data transmission, and user-friendly platforms. In some rural or underserved areas, the lack of adequate technology infrastructure can hinder the adoption of telemedicine.
Regulatory and Licensing Issues
Telemedicine involves navigating a complex landscape of regulatory and licensing issues. Different states and countries have varying regulations regarding telemedicine practices, reimbursement policies, and patient privacy. Healthcare providers must ensure compliance with these regulations to avoid legal and financial repercussions.
Patient and Provider Acceptance
The acceptance of telemedicine by both patients and providers is crucial for its success. Some patients may be hesitant to adopt telemedicine due to concerns about privacy, data security, or the perceived impersonal nature of virtual consultations. Similarly, healthcare providers may be resistant to change or lack the necessary training to effectively use telemedicine platforms.
Ensuring Quality of Care
Maintaining the quality of care in telemedicine is another important consideration. While telemedicine can enhance access to specialty care, it is essential to ensure that virtual consultations are as effective as in-person visits. This requires robust protocols, continuous training, and the use of advanced diagnostic tools to support remote assessments.
Conclusion
Telemedicine is transforming the landscape of specialty care, offering a range of benefits that enhance access, efficiency, and quality of care. By bridging geographical gaps, reducing wait times, and expanding access to expertise, telemedicine is making specialized medical services more accessible to patients across the globe. For healthcare providers, telemedicine offers opportunities for increased efficiency, professional collaboration, and financial growth.
However, to fully harness the potential of telemedicine in specialty care, it is essential to address the challenges related to technology, regulation, acceptance, and quality of care. By doing so, we can create a more inclusive and effective healthcare system that leverages the power of digital technology to improve health outcomes for all.
Beauty Fitness
Liposuction: Cheap vs Premium Clinics for Effective Results

Liposuction in Islamabad is becoming increasingly popular among people looking to achieve a slimmer body. With many clinics offering varying prices, it’s essential to understand the difference between cheap and premium options. Your choice can affect both the results and your safety.
Understanding Cheap Liposuction in Islamabad
Cheap Liposuction in Islamabad is often chosen by patients looking for affordable ways to remove stubborn fat. The lower cost can make the procedure appealing, especially for those on a tight budget. However, it’s important to understand what “cheap” really means in this context. Often, these procedures may use older equipment or be performed in clinics with less experienced staff.
While cheap Liposuction in Islamabad can deliver results, the quality of care and safety may not match premium clinics. There is a higher chance of complications such as uneven fat removal, infection, or longer recovery periods. Patients should carefully research the clinic, check surgeon qualifications, and read patient reviews before deciding.
Natural ways to prepare for surgery, such as maintaining a balanced diet and regular exercise, can improve outcomes regardless of the clinic you choose. Aftercare is equally important, but some budget clinics may not provide comprehensive guidance.
In short, cheap Liposuction in Islamabad can be an option for those mindful of costs, but safety and results should remain a priority. Investing time in research and preparation ensures you achieve better outcomes while minimizing risks.
Premium Liposuction in Islamabad
Premium Liposuction in Islamabad offers advanced technology and highly trained surgeons. Clinics offering premium services provide a safer environment and personalized care. The procedure usually results in smoother outcomes and faster recovery. While more expensive, the long-term benefits are often worth the investment.
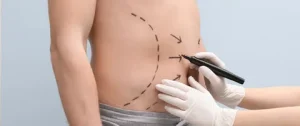
Key Differences Between Cheap and Premium Liposuction
Here are some major points to consider when choosing between cheap and premium Liposuction in Islamabad:
- Cost vs Safety: Cheap options save money but may compromise on safety.
- Experience of Surgeons: Premium clinics employ certified, experienced professionals.
- Equipment Quality: Advanced tools in premium clinics ensure better results.
- Aftercare Support: Premium clinics provide structured follow-up for recovery.
- Hospital Standards: Higher-end clinics follow strict hygiene and safety standards.
Why Cost Shouldn’t Be the Only Factor
While affordable Liposuction in Islamabad is tempting, focusing solely on cost can be risky. Quality of care, surgeon expertise, and clinic standards directly impact your results. Natural ways to prepare for surgery, like maintaining a healthy diet and exercise routine, can improve outcomes regardless of the clinic you choose.
Recovery and Aftercare
Recovery and aftercare are crucial steps following Liposuction in Islamabad to ensure safe healing and optimal results. After the procedure, patients may experience swelling, bruising, or mild discomfort. These are normal and usually subside within a few weeks. Following your surgeon’s instructions is essential to minimize complications and achieve the desired outcome.
Most premium clinics recommend wearing compression garments to support the treated areas. These garments help reduce swelling and contour the body shape. Pain management is also important, and your doctor may prescribe mild medications to ease discomfort. Regular check-ups during the first few weeks allow the surgeon to monitor healing progress.
Incorporating natural ways to enhance recovery can be very effective. Eating a balanced diet, staying hydrated, and engaging in light physical activity, such as short walks, can boost circulation and aid in faster healing. Avoiding smoking and alcohol is highly recommended as they can slow down the recovery process.
Proper aftercare also involves maintaining hygiene around the incision sites and promptly reporting any unusual symptoms to your surgeon. Choosing a reputable clinic ensures structured guidance, making your Liposuction in Islamabad experience safer and more satisfying.
Choosing the Right Clinic
Selecting the right clinic for Liposuction in Islamabad requires research. Look for reviews, surgeon credentials, and patient testimonials. Visiting the clinic before surgery helps you understand the environment and professionalism. Investing in a reputable clinic ensures your safety and satisfaction with the results.
FAQs About Liposuction in Islamabad
Q1: Is cheap liposuction safe?
A1: While possible, cheap Liposuction in Islamabad often carries higher risks due to older equipment or less experienced surgeons.
Q2: How long is the recovery time?
A2: Recovery usually takes 2–4 weeks, but premium clinics provide better guidance to speed up healing.
Q3: Can natural ways improve liposuction results?
A3: Yes, healthy diet, light exercise, and hydration help enhance results and reduce complications.
Q4: How do I choose between cheap and premium options?
A4: Evaluate clinic reputation, surgeon experience, equipment quality, and aftercare before deciding.
Q5: Are the results permanent?
A5: Liposuction in Islamabad provides long-lasting results if a stable lifestyle and natural ways of maintaining weight are followed.
Final Thoughts
Choosing between cheap and premium Liposuction in Islamabad is about balancing cost and safety. Prioritizing quality ensures better results, faster recovery, and minimal risk. For those seeking the best care and outcomes, trusted clinics like skn cosmetics offer professional services that meet international standards.
Care
Top Reasons Adults Choose Hormone Replacement Services in Houston
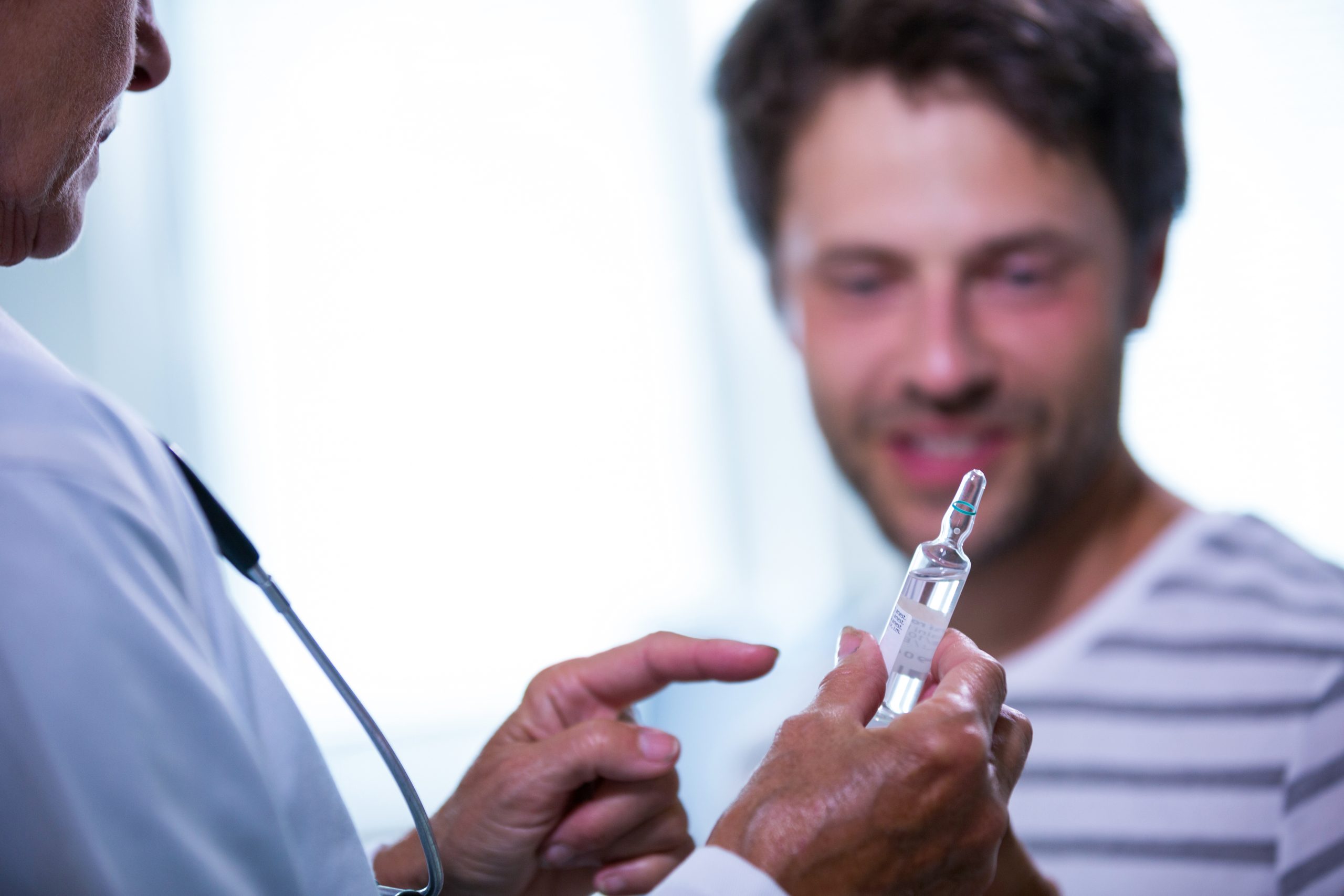
Hormone changes are a normal part of aging. As you get older, your body may not produce hormones at the same levels as before. These shifts can affect how you feel day-to-day, including your energy, sleep, mood, and focus. Many adults living in Houston begin to notice these changes and look for ways to better understand what is happening in their bodies.
Some people try to adjust their lifestyle first. They may improve their diet, exercise more, or work on sleep habits. While these steps are helpful, they do not always address hormone-related concerns fully. This is where structured evaluation and care can help.
Hormone-focused services look at your symptoms and lab test results to understand your body more fully. Instead of guessing, you receive information based on measurable data. This helps guide decisions and next steps in a clearer and more practical manner.
Key Reasons Adults Turn to Hormone Replacement in Houston Care
-
Addressing low energy that affects daily life
Many adults feel tired even after enough sleep, which can affect daily tasks and focus. Hormones such as thyroid hormone and testosterone help regulate energy levels. When these hormones are out of balance, you may feel drained without a clear reason.
Testing helps determine whether hormones are the cause, and care plans can then include hormone support, along with routine and nutrition guidance, to address the root issue rather than just the symptoms.
-
Supporting mood changes and mental clarity
Hormones influence brain function, including mood and concentration. When levels shift, you may notice irritability, stress, or difficulty staying focused.
These changes can affect your relationships, work, and overall quality of life. By reviewing hormone levels, a provider can look for patterns that may explain these symptoms. In some cases, adjusting hormone levels may help support more stable mood and clearer thinking.
This process is often combined with lifestyle habits such as regular sleep, balanced meals, and stress management techniques.
-
Managing natural hormone decline with age
Hormone levels change as part of the aging process. This happens in both men and women, although the patterns may differ.
For example, testosterone levels may decrease in men over time, while women may experience changes in estrogen and progesterone. These shifts can bring noticeable symptoms that develop slowly.
Regular evaluation helps track these changes over time. With ongoing monitoring, you and your provider can make informed decisions about whether support is needed and how to adjust care as your body changes.
-
Improving sleep quality and patterns
Sleep issues are often linked to hormone imbalance. Hormones such as cortisol and melatonin help regulate your sleep cycle.
If these hormones are out of balance, you may find it hard to fall asleep or stay asleep through the night. Poor sleep can then affect energy, mood, and overall health.
In cases where sleep problems are linked to hormones, evaluation can help identify the cause. Care may include hormone-related support, along with habits such as maintaining a consistent sleep schedule, limiting screen time before bed, and creating a calm sleep environment.
-
Supporting weight management efforts
Weight changes can be influenced by hormone levels. Hormones help regulate metabolism, appetite, and fat storage.
Some adults follow diet and exercise routines but still find it difficult to manage their weight. In these situations, hormone testing may provide more insight into what is happening inside the body.
A provider may review hormones related to metabolism, such as thyroid hormones and insulin. Based on the results, a plan may include a mix of hormone support, nutrition guidance, and physical activity recommendations.
-
Improving physical performance and recovery
Hormones also play a role in muscle strength, endurance, and recovery after exercise.
If your hormone levels are not balanced, you may notice reduced performance during workouts or longer recovery times. This can make it harder to stay consistent with fitness routines.
By checking hormone levels, providers can identify areas that may be affecting your physical performance. With proper guidance, you may see improvements in strength, stamina, and recovery when combined with regular exercise and proper rest.
-
Personalized care with ongoing monitoring
One main reason adults choose hormone-related services is the structured, personalized approach. Care is not a one-time visit. It usually includes consultation, lab testing, a tailored plan, follow-ups, and adjustments based on progress.
This step-by-step process helps track changes over time and ensures care is updated based on how your body responds. When considering options like hormone replacement in Houston, many adults prefer services that combine testing, guidance, and ongoing support for a clearer path forward.
Summary!
Hormone-related concerns can affect many areas of daily life, including energy, sleep, mood, weight, and physical performance. As these changes develop over time, it can be helpful to look at your health in a structured way that includes both testing and ongoing evaluation.
Choosing hormone-focused care allows you to better understand what is happening inside your body and take informed steps based on real data. With the right approach, you can work toward better balance while maintaining your daily routine and lifestyle.
In Houston, PUUR Health and Wellness offers a care model that focuses on personalized evaluation, monitoring, and guided support. This type of approach helps you move forward with clarity and consistent follow-up as part of your overall wellness plan.
Care
Ayurvedic Retinitis Pigmentosa Treatment: Holistic Eye Care

Living with retinitis pigmentosa (RP) can feel like an uphill battle. Everyday tasks that once seemed simple slowly become more challenging. You might struggle to see in dim light or notice that your peripheral vision is narrowing. These changes often create a significant amount of stress and anxiety. It is perfectly natural to feel overwhelmed when you are unsure about what the future holds for your sight.
In the United States, many people with RP are searching for ways to manage their condition beyond standard clinical care. While modern medicine excels at tracking the progression of the disease, it does not always provide long-term solutions to slow it down. This gap in care is why Ayurveda is gaining so much attention as a supportive option.
Ayurveda focuses on creating balance within your body and your daily habits. Instead of looking for a “quick fix,” this ancient system emphasizes steady and consistent care. In this comprehensive guide, we will explore how Ayurvedic principles can fit into your life as you manage the complexities of RP.
Understanding Your Condition and Setting Realistic Goals
Before you begin any new health regimen, you must understand exactly what RP is. It is a genetic condition that affects the retina’s ability to respond to light. Because it is hereditary, its effects vary wildly from person to person. Some individuals experience a very slow decline over decades. Others may see faster changes in their visual field.
Ayurveda encourages you to set realistic expectations from the start. You should not view this as an instant cure. Instead, you are working toward sustainable goals. These include maintaining your current level of vision, reducing daily ocular discomfort, and supporting the long-term health of your eye tissues. When you adopt this mindset, staying consistent with your care plan becomes much easier. It also helps lower your anxiety because you are focusing on what you can control today.

Supporting Your Body as a Complete System
Ayurveda does not view your eyes as isolated organs. Instead, it connects your vision to the overall balance of your entire body. According to this philosophy, your eyes depend on healthy digestion, efficient circulation, and strong nerve function. If one part of the system falters, the eyes feel the impact.
This is why an Ayurvedic approach to retinitis pigmentosa treatment often includes:
-
Herbal Supplements: These formulas support specific bodily functions like blood flow and cellular repair.
-
Gentle Detoxification: This process removes metabolic waste that might hinder your systemic health.
-
Customized Diet Plans: A specialized diet helps improve your “digestive fire,” ensuring your eyes get the nutrients they need.
Many people in the U.S. are now exploring this holistic approach. They appreciate that it looks at long-term wellness rather than just masking symptoms. By helping your body function better as a whole, you provide your eyes with a much stronger foundation for health.
Using Targeted Ayurvedic Eye Therapies
Ayurveda also offers specific treatments that focus directly on the ocular area. You should always undergo these therapies under the supervision of a trained professional. These methods aim to nourish the delicate tissues of the eye and soothe the optic nerve.
One commonly used method is Netra Tarpana. In this therapy, a practitioner applies medicated ghee (clarified butter) around the eyes for a set period. This process deeply hydrates the area and helps reduce the strain of constant squinting. Other techniques include gentle herbal cleansing to remove surface irritants and external herbal poultices.
While these therapies cannot reverse the genetic coding of RP, they can significantly improve how your eyes feel on a daily basis. They help reduce dryness, itching, and redness. Consistency is the secret to success here. You might not see a change after one session, but a structured plan often yields noticeable results over several months.
Making Simple Lifestyle Changes for Maximum Impact
Your daily routine plays a massive role in how you manage a chronic condition like RP. Ayurveda places heavy importance on simple, grounding habits. These small steps may seem basic, but they create a cumulative effect on your well-being.
You can start by auditing your kitchen. Prioritize fresh, home-cooked meals over processed or packaged foods. Processed items often contain preservatives that can cause systemic inflammation. Additionally, try to sleep at the same time every night. A regular sleep schedule allows your body to enter a deep state of repair.
Furthermore, you should limit your screen time whenever possible. Blue light from phones and computers can strain already sensitive retinas. You can also incorporate light eye exercises and relaxation techniques. Simple breathing exercises and daily meditation help reduce cortisol levels. Lowering stress is vital because high stress can negatively impact your overall immune response and eye health.
Combining Ayurveda with Modern Eye Care
You do not have to choose between ancient wisdom and modern science. In fact, many people find the most success when they combine both. This “integrative” approach allows you to get the best of both worlds. You can use modern technology to monitor the physical changes in your retina while using Ayurveda to support your body naturally.
With this balanced combination, you can:
-
Track Progress: Continue regular check-ups with your ophthalmologist to monitor vision changes accurately.
-
Follow a Plan: Stick to a structured Ayurvedic routine to keep your internal systems balanced.
-
Adjust as Needed: Work with both your doctor and your Ayurvedic practitioner to tweak your treatments based on your actual progress.
This proactive stance helps you feel more in control of your health. It moves you from a passive observer of your condition to an active participant in your care.
Conclusion: A Path Toward Consistent Care
Living with retinitis pigmentosa can certainly feel overwhelming at times. However, having a structured and compassionate approach can make a world of difference. Ayurveda offers a unique way to support your body through steady and intentional care. It prioritizes balance, routine, and long-term vitality over temporary results.
By understanding your condition deeply, making simple lifestyle adjustments, and exploring guided therapies, you can manage your daily life more effectively. Thousands of people are now adding Ayurveda to their care plans to improve their comfort and support their overall ocular health.
Organizations like the Netra Eye Institute are leading the way in this field. They provide structured programs that combine traditional Ayurvedic methods with a modern understanding of eye diseases. This type of comprehensive support helps you navigate the challenges of RP with more confidence and peace of mind. Remember, the goal is not to find a miracle but to build a lifestyle that protects and nourishes your vision for as long as possible. Starting today with small, consistent changes can lead to a much brighter future for your eye health.
-
Business3 years ago
Cybersecurity Consulting Company SequelNet Provides Critical IT Support Services to Medical Billing Firm, Medical Optimum
-
Business3 years ago
Team Communication Software Transforms Operations at Finance Innovate
-
Business3 years ago
Project Management Tool Transforms Long Island Business
-
Business3 years ago
How Alleviate Poverty Utilized IPPBX’s All-in-One Solution to Transform Lives in New York City
-
health3 years ago
Breast Cancer: The Imperative Role of Mammograms in Screening and Early Detection
-
Sports3 years ago
Unstoppable Collaboration: D.C.’s Citi Open and Silicon Valley Classic Unite to Propel Women’s Tennis to New Heights
-
Art /Entertainment3 years ago
Embracing Renewal: Sizdabedar Celebrations Unite Iranians in New York’s Eisenhower Park
-
Finance3 years ago
The Benefits of Starting a Side Hustle for Financial Freedom