health
Don’t Wait Until You’re Sick: Proactive Health Hacks for Everyone

Meet Dr. Sarah Jones!
Dr. Sarah Jones is a passionate family physician with over 10 years of experience in preventative medicine. Dedicated to empowering her patients, Dr. Jones believes everyone can achieve optimal health through proactive measures. In this informative guide, Dr. Jones shares her top tips for taking control of your well-being, so you can stay healthy and vibrant for years to come!
Why Wait? The Power of Preventative Healthcare
Think of your health like a car. Regular maintenance – oil changes, tire rotations, tune-ups – keeps it running smoothly and prevents costly breakdowns down the road. The same goes for your body! Preventative healthcare is all about taking proactive steps to safeguard your well-being and minimize the risk of future health problems.
Taking Charge: Your Personalized Health Toolkit
The good news? You hold the key to unlocking a healthier, happier you! By incorporating a few simple strategies into your daily routine, you can significantly improve your overall health and well-being. Here, Dr. Jones equips you with your personalized health toolkit:
Diet & Nutrition: Fueling Your Body for Success
Just like a high-performance car needs premium fuel, your body thrives on a balanced diet rich in essential nutrients. Focus on consuming plenty of fruits, vegetables, and whole grains. Lean protein sources like fish, chicken, and beans provide the building blocks for strong muscles and tissues. Don’t forget healthy fats – avocados, nuts, and olive oil – essential for brain function and hormone regulation.
Tip: Planning your meals and snacks in advance can help you avoid unhealthy choices when hunger strikes.

Picture by: https://bocaratondentalsleepmedicine.com/blog/2021/01/i-sleep-alone-how-can-i-tell-if-i-have-sleep-apnea/
Move It or Lose It: The Importance of Exercise
Regular physical activity is a cornerstone of good health. Exercise strengthens your heart and lungs, boosts your mood, and helps manage weight. Aim for at least 150 minutes of moderate-intensity exercise or 75 minutes of vigorous-intensity exercise each week.
Key point: Find activities you enjoy – dancing, swimming, biking – to make exercise a fun and sustainable part of your life.
Sleep Well, Live Well: Prioritizing Restful Nights
Quality sleep is vital for both physical and mental health. When you sleep, your body repairs itself, consolidates memories, and regulates hormones. Most adults require 7-8 hours of sleep per night.
Actionable Step: Establish a relaxing bedtime routine to wind down before sleep, including dimming lights and avoiding screens for at least an hour before bed.
Mind Over Matter: The Link Between Stress and Health
Chronic stress can wreak havoc on your health, increasing your risk for heart disease, diabetes, and even depression. Techniques like yoga, meditation, and deep breathing can help manage stress and promote relaxation.
Know Your Numbers: Regular Checkups and Screenings
Schedule regular checkups with your doctor, even when you feel healthy. These visits allow for early detection of potential health issues, enabling prompt treatment and improved outcomes. Don’t forget about age-appropriate screenings for conditions like cancer, diabetes, and high blood pressure.
Building a Healthy Routine: Habits for Lifelong Wellness
The key to lasting health improvements lies in creating sustainable habits. Start small and gradually incorporate these health hacks into your daily routine. Remember, consistency is key!
Beyond the Basics: Tailoring Your Approach
While these tips provide a solid foundation, Dr. Jones acknowledges that a one-size-fits-all approach doesn’t work for everyone. Consider consulting a registered dietitian for personalized dietary advice or a certified personal trainer to develop a safe and effective exercise program.
Care
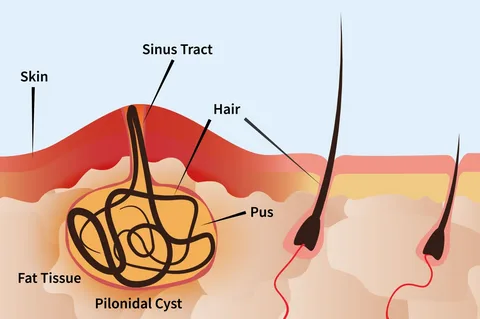
Pilonidal Sinus Treatment: Causes, Symptoms, and Laser Care
Equipments
Thumb Tissue Forceps: Engineering for Surgical Excellence

Control, accuracy, and tissue protection are central to every successful procedure. Among the many handheld instruments used in the operating room, thumb tissue forceps play a vital role in helping surgeons grasp, stabilize, and manipulate tissue with confidence. Their thumb tissue forceps simple form hides a highly refined design that supports delicate work across many surgical fields.
Role of Tissue Forceps in Surgery
In daily surgical practice, forceps are more than basic grasping tools. They act as extensions of the surgeon’s hand, allowing precise handling of skin, fascia, vessels, and other soft tissue structures. The ability to secure tissue without causing unnecessary trauma can influence visibility, efficiency, and overall surgical outcomes. Thumb tissue forceps are designed for manual control through direct finger pressure rather than ring handles or locking mechanisms.
This design gives the operator immediate tactile response, which is essential when working with fragile or mobile tissue. In procedures where precision must be maintained at every moment, this responsive handling becomes a major clinical advantage.
Key Technical Specifications
The performance of any surgical instrument depends on its technical details. Tissue forceps are commonly manufactured in high-grade surgical stainless steel to provide corrosion resistance, strength, and compatibility with repeated autoclave cycles. Material quality is essential because even minor deformation at the tip can reduce alignment and compromise handling accuracy. Tip configuration is another critical specification.
Some magill forceps use models feature fine serrations for improved grip, while others include delicate teeth that allow secure tissue engagement with minimal slippage. Length also matters, as shorter instruments may support finer control in superficial procedures, while longer designs help improve access in deeper operative fields. Spring tension must be carefully balanced so the instrument opens smoothly yet closes with enough force to maintain tissue control without excessive hand fatigue.
Precision Engineering
Precision engineering is the defining factor that separates a routine instrument from one that performs consistently in demanding surgical settings. The most effective forceps are manufactured with close tolerances to ensure exact tip alignment, even pressure distribution, and dependable closure. When the tips meet perfectly, surgeons can grasp tissue more accurately and reduce the risk of tearing or crushing delicate structures.
This level of refinement also supports procedural efficiency. Poorly aligned tips can interrupt surgical flow, force repeated repositioning, and increase frustration during critical moments. Grey Medical emphasizes precision-crafted design because surgical professionals require instruments that respond predictably under pressure. In microsurgical, general, plastic, and vascular environments, dependable engineering is not a luxury. It is a requirement.
Surgical Applications Across Specialties
The versatility of thumb tissue forceps makes them useful in a broad range of procedures. In general surgery, they assist with holding tissue edges, supporting dissection, and improving exposure in both minor and major operations. In plastic and reconstructive surgery, the ability to handle tissue delicately is especially valuable where cosmetic and structural outcomes depend on minimizing trauma.
These instruments are also widely used in dermatologic, ENT, gynecologic, and vascular procedures. In each specialty, the surgeon relies on consistent grip and tactile sensitivity to perform exact movements. Whether handling fine skin margins during closure or stabilizing tissue for suturing, the instrument must support precision without compromising tissue integrity. That balance is central to high-quality surgical care.
Tissue Handling and Atraumatic Performance
One of the most important concerns in instrument design is how the tool interacts with living tissue. Excess pressure, rough serrations, or poor tip finish can cause avoidable trauma. For this reason, the geometry of the forceps tips must be matched to the intended tissue type and surgical task. Instruments used for delicate structures require finer contact surfaces and refined gripping patterns.
Well-designed thumb tissue forceps help maintain control while reducing slip and minimizing crush injury. This is particularly important during procedures that demand gentle approximation, careful traction, or exact suturing support. Surgeons often judge an instrument not only by how well it grips, but by how safely it releases tissue after contact. A smooth, precise finish contributes directly to that performance.
Durability, and Reliability
Surgical instruments must perform repeatedly in environments where there is no room for inconsistency. They are exposed to frequent cleaning, chemical processing, mechanical handling, and high-temperature sterilization. Any weakness in material selection or manufacturing can shorten service life and affect clinical reliability. A quality instrument must maintain its spring action, surface integrity, and tip precision over time.
This is where trusted manufacturing standards become essential. Grey Medical focuses on premium-quality surgical instruments because medical professionals need equipment that holds up under real operating conditions. Long-term reliability supports not only cost efficiency, but also patient safety and workflow consistency. When an instrument maintains its original function after repeated use, it becomes a dependable part of the surgical set rather than a variable risk.
Instrument Quality Influences Surgical Outcomes
Instrument quality has a direct effect on how a procedure feels and flows in the surgeon’s hand. Smooth action, accurate grip, and stable tip engagement contribute to better control in every phase of tissue handling. When a surgeon can rely on the instrument, attention remains focused on anatomy and technique rather than tool adjustment. That confidence supports both speed and precision in the operating field.
For this reason, thumb tissue forceps should never be treated as a generic accessory. Their design influences tissue preservation, visibility, and hand comfort during repetitive use. In specialties where precision defines results, the right instrument helps reduce handling error and supports better procedural consistency. High standards in manufacturing are therefore closely linked to high standards in care.
Conclusion
Surgical excellence depends on instruments that combine technical accuracy, ergonomic control, and durable construction. From tip alignment and spring tension to material quality and atraumatic handling, every detail matters when selecting forceps for professional use. These instruments may appear simple, but their performance has a meaningful effect on surgical efficiency and tissue safety.
Grey Medical brings decades of medical industry experience to the development of precision-crafted tools for surgeons and healthcare professionals worldwide. By focusing on engineering quality and dependable performance, the company supports the demanding standards of modern operating rooms. For professionals seeking thumb tissue forceps that reflect precision, consistency, and surgical reliability, Grey Medical remains a trusted partner in advanced instrument selection.
Beauty Fitness
Immune Boost IV Drip: Benefits, Process, and Wellness Essential
In the fast-paced world of 2026, maintaining peak health is a top priority for residents in the UAE. The Immune Boost IV Drip in Dubai has evolved into a vital medical tool for those who value efficiency. While many people rely on oral vitamins, clinical evidence shows that intravenous therapy offers superior results. By delivering nutrients directly into your bloodstream, this treatment ensures your body receives the full benefit of every vitamin. It is the gold standard for anyone looking to strengthen their natural defenses against the stressors of urban life.
Immune Boost IV Drip in Dubai
A medical IV drip is more than just a hydration tool. It is a precise blend of pharmaceutical-grade micronutrients. The Immune Boost IV Drip in Dubai typically contains high doses of Vitamin C, Zinc, and B-complex vitamins. It also often includes Glutathione, which is the body’s most powerful antioxidant.
Treatment Strengthens Your Body
The science behind the Immune Boost IV Drip in Dubai focuses on cellular saturation. When the concentration of vitamins in your blood rises, your cells can absorb them more effectively. This surge in nutrients triggers several positive biological responses.
First, the infusion rehydrates your body at a deep cellular level. This is crucial in the arid climate of Dubai, where dehydration can weaken your mucosal barriers. Second, the high dose of Vitamin C empowers your white blood cells. These cells act as your body’s primary soldiers against viruses. Finally, the electrolytes in the saline solution restore your internal balance. This helps you recover from the physical exhaustion that often leads to illness.
Choosing Clinical IV Therapy
Many professionals in Dubai choose this therapy as a proactive measure. It serves a specific purpose in a high-demand environment.
-
Fast Recovery: It shortens the duration of seasonal colds or flu symptoms.
-
Travel Readiness: It protects frequent flyers from germs in crowded airports.
-
Stress Management: It replenishes the nutrients that your body burns through during high-pressure work weeks.
-
Systemic Detox: It helps the liver filter out pollutants and metabolic waste.
Benefits for Your Health and Vitality
Choosing an Immune Boost IV Drip in Dubai provides systemic benefits that improve your daily life. Most patients notice an immediate lift in their mood and energy levels.
The most significant benefit is the rapid increase in viral resistance. Because the nutrients are already in your blood, your immune response becomes much faster. Additionally, the antioxidants in the drip help reduce systemic inflammation. This can lead to better sleep quality and clearer skin. Furthermore, the B-vitamins in the formula support your brain health. This ensures you stay focused and productive throughout your busy schedule.
The Procedure
-
Medical Consultation: A licensed professional reviews your health history and checks your vital signs.
-
Custom Mixing: The Immune Boost IV Drip in Dubai is prepared using sterile, high-potency ingredients.
-
Quick Placement: A nurse inserts a tiny, flexible tube into a vein in your arm with very little discomfort.
-
Relaxing Infusion: You rest in a comfortable chair for about 45 minutes while the drip works.
-
Post-Care Review: The nurse removes the tube and provides tips on how to maintain your energy boost.
Impact on Your Biological Target Zones
Once the nutrients enter your system, they head straight to where they are needed most. The Immune Boost IV Drip in Dubai targets your lymphatic system first. This system is responsible for moving immune cells around your body. Next, the vitamins reach your adrenal glands. These glands control your stress hormones. By supporting these specific areas, the drip helps “reset” your internal clock. As a result, you feel more resilient and less prone to the “burnout” that many residents experience.
Cost and Medical Standards in Dubai
The cost of an Immune Boost IV Drip in Dubai reflects the quality of the medical care you receive. At a professional clinic, you pay for pharmaceutical-grade ingredients and expert supervision. It is important to avoid low-quality “wellness bars” that do not follow strict medical guidelines. A licensed facility ensures that your drip is safe and effective. Therefore, investing in a clinical-grade drip is the best way to guarantee a therapeutic result for your health.
Expect During Your Recovery
There is no downtime after an IV session. You can walk out of the clinic and return to your normal routine immediately.
Safety Protocols and Clinical Integrity
Safety is our top priority for every patient. Before we administer an Immune Boost IV Drip in Dubai, we perform a thorough screening. We check for allergies and ensure your kidneys are functioning well. While side effects are very rare, they are usually limited to small bruises at the injection site. By following these strict 2026 medical protocols, we provide a wellness experience that is both comfortable and secure.
Tips for Maintaining Your Results
To make the most of your Immune Boost IV Drip in Dubai, you should follow a few simple steps.
First, continue to drink plenty of water. Hydration helps your kidneys process the vitamins effectively. Second, try to get at least seven hours of sleep. Your body does its best repair work while you rest. Finally, eat a balanced diet full of fresh vegetables. These healthy habits work together with the IV drip to keep your immune system in top shape for the long term.
Conclusion
Your health is the foundation of your success. By choosing an Immune Boost IV Drip in Dubai, you are taking a proactive step to protect your future. At Tajmeels Clinic, we combine medical expertise with personalized care to help you feel your best. We believe that everyone deserves access to high-quality cellular support. Whether you want to avoid a cold or simply boost your energy, we are here to help you reach your goals. Invest in your resilience today with the power of professional IV therapy.
-
Business3 years ago
Cybersecurity Consulting Company SequelNet Provides Critical IT Support Services to Medical Billing Firm, Medical Optimum
-
Business3 years ago
Team Communication Software Transforms Operations at Finance Innovate
-
Business3 years ago
Project Management Tool Transforms Long Island Business
-
Business3 years ago
How Alleviate Poverty Utilized IPPBX’s All-in-One Solution to Transform Lives in New York City
-
health3 years ago
Breast Cancer: The Imperative Role of Mammograms in Screening and Early Detection
-
Sports3 years ago
Unstoppable Collaboration: D.C.’s Citi Open and Silicon Valley Classic Unite to Propel Women’s Tennis to New Heights
-
Art /Entertainment3 years ago
Embracing Renewal: Sizdabedar Celebrations Unite Iranians in New York’s Eisenhower Park
-
Finance3 years ago
The Benefits of Starting a Side Hustle for Financial Freedom