health
The Brave Little Fighters: Understanding the Unique Challenges of Childhood Cancer

Childhood cancer is a topic that touches the hearts of many. It’s difficult to think about innocent children facing such a challenging and life-altering illness. However, it’s important to understand the unique challenges that these brave little fighters face every day. From their treatment plans to their emotional well-being, childhood cancer presents its own set of obstacles that require attention and understanding. In this blog post, we’ll explore what makes childhood cancer so different from other illnesses, and how we can support these young warriors in their fight against cancer.
What is Childhood Cancer?
Childhood cancer is a type of cancer that affects children. It is the leading cause of death by disease in children under the age of 15. There are many types of childhood cancers, but the most common are leukemia, brain tumors, and lymphoma.
Childhood cancer is different from adult cancer in many ways. The biggest difference is that children’s bodies are still growing and developing, so the cancer can grow faster and spread to other parts of the body more easily. Children also have a higher risk of developing certain types of cancers, such as leukemia, than adults do.
Treatment for childhood cancer is also different from adult cancer treatment. Children’s bodies are more sensitive to the side effects of chemotherapy and radiation therapy, so these treatments are often given at lower doses. Surgery is also often used to treat childhood cancers, as it is less likely to cause long-term side effects than radiation or chemotherapy.
The survival rates for childhood cancer have improved dramatically over the past few decades. The overall five-year survival rate for all childhood cancers is now 80%, and it is even higher for specific types of cancers such as leukemia (89%) and brain tumors (94%). However, there is still much room for improvement, as many children with cancer still do not survive their disease.
The Different Types of Childhood Cancer
There are many different types of childhood cancer, each with its own set of unique challenges. The most common type of childhood cancer is leukemia, which accounts for about 30% of all cases. Other common types include brain tumors, lymphoma, and solid tumor cancers.
Each type of childhood cancer has its own set of symptoms and treatment options. Leukemia, for example, is typically treated with chemotherapy. Brain tumors may be treated with surgery, radiation therapy, or both. Lymphoma may be treated with radiation therapy or chemotherapy. And solid tumor cancers may be treated with surgery, radiation therapy, or a combination of both.
The prognosis for each type of childhood cancer varies depending on the specific diagnosis. In general, however, survival rates for all types of childhood cancer have been increasing in recent years thanks to advances in medical research and treatment options.
The Causes of Childhood Cancer
There are many different types of childhood cancers, and each has its own set of causes. In general, cancer is caused by the abnormal growth of cells in the body. This can happen as a result of a genetic mutation, exposure to certain environmental factors, or a combination of both.
Some specific causes of childhood cancer include:
• Exposure to ionizing radiation: This type of radiation is found in X-rays, CT scans, and other medical imaging procedures. It can also come from nuclear power plants and other sources. Studies have shown that children who are exposed to ionizing radiation are at an increased risk for developing leukemia and brain tumors.
• Chemicals: Children who are exposed to certain chemicals, such as benzene and pesticides, may be more likely to develop cancer.
• Infections: Some viruses and bacteria can increase the risk for developing certain types of childhood cancers, such as leukemia and lymphoma.
• Genetic mutations: Certain genetic mutations can be passed down from parents to children and increase the risk for developing cancer.
The Symptoms of Childhood Cancer
There are a number of different symptoms that can indicate childhood cancer. Some of the more common ones include:
– Persistent fevers that don’t respond to medication
– Unexplained weight loss or poor appetite
– Fatigue or lethargy
– Pain in the bones or joints
– Lumps or swellings anywhere on the body
– easy bruising or bleeding
– Recurrent infections
– Abnormalities with the eyes, such as redness, swelling, or discharge
The Treatment of Childhood Cancer
Though cancer in children is rare, accounting for less than 1% of all cancers diagnosed annually in the United States, it is the leading cause of death by disease in children under the age of 15.
There are many types of childhood cancer, and each requires its own unique treatment plan. In general, though, treatment will involve a combination of surgery, radiation therapy, and/or chemotherapy. The specific approach will be determined by the child’s age, overall health, and the type and stage of cancer.
Childhood cancer can be a very difficult thing for a family to deal with. Not only is it emotionally devastating to watch your child suffer, but it can also be financially ruinous. The good news is that there are many organizations dedicated to helping families dealing with childhood cancer. These organizations can provide financial assistance, emotional support, and practical help with day-to-day tasks.
The Unique Challenges of Childhood Cancer
Cancer is a scary diagnosis at any age, but it can be especially frightening for children. Not only are they faced with a potentially life-threatening illness, but they must also deal with the side effects of treatment, which can be both physically and emotionally challenging.
In addition to the physical challenges, childhood cancer can also take an emotional toll on patients and their families. The diagnosis can be overwhelming and scary, and treatment can be long and difficult. Children with cancer often miss out on important milestones like school graduation or prom, and they may feel isolated from their friends. Families may also struggle with the financial burden of treatment, as well as the emotional roller coaster of watching their child go through such a tough experience.
But despite all of these challenges, childhood cancer patients are brave little fighters. They show tremendous courage in the face of adversity, and they inspire us all to never give up hope.
Conclusion
Childhood cancer is a heartbreaking experience for families and communities alike. We must never forget the brave little fighters who courageously face this unique challenge every single day, and we must do all that we can to support them. With knowledge of the different types of childhood cancer, their risk factors, and the treatments available, we can start to take meaningful steps towards improving outcomes with these courageous children in our lives. Let’s stand together against childhood cancer and give these young warriors the strength they need to beat this horrible disease!
Beauty Fitness
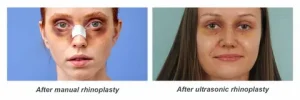
Ultrasonic Rhinoplasty: Precision, Innovation, and Rapid Recovery
In the high-velocity world of global commerce, where Riyadh stands as a central pillar of innovation and investment, time is the ultimate luxury. For the modern executive, diplomat, or entrepreneur, the decision to undergo a personal refinement procedure is often weighed against the potential for professional disruption. In the pursuit of “Sovereign Excellence,” a leader’s physical presence must reflect their internal discipline and authority, yet the demands of a high-stakes career leave little room for traditional recovery periods. This is why many professionals are now choosing Ultrasonic Rhinoplasty, which offers greater precision and significantly reduced downtime compared to conventional surgical methods.
This is why the elite of the Kingdom are increasingly turning to a technological revolution that balances aesthetic perfection with surgical efficiency. Ultrasonic Rhinoplasty in Riyadh has been transformed by the introduction of Ultrasonic (Piezo) technology, a breakthrough that provides a “Rapid ROI” by significantly minimizing downtime while maximizing the precision of the results.
The Executive Dilemma
For decades, the primary barrier to nasal refinement for high-profile individuals was the “social tax” associated with traditional surgery. Conventional methods relied on mechanical force—using hammers and chisels—to reshape the nasal bones. This blunt-force approach inevitably caused significant trauma to the surrounding soft tissues, delicate blood vessels, and nerves. The result for the patient was a period of intense bruising and swelling that could last for weeks, making it impossible to attend board meetings, public summits, or international negotiations without revealing the surgical journey.
Science of the “Quiet Recovery”
Ultrasonic Rhinoplasty, or Piezo surgery, represents a paradigm shift from the mechanical to the micrometric. Instead of manual instruments, surgeons use high-frequency sound waves to sculpt the nasal architecture. This technological edge provides several key advantages that directly contribute to a faster “Return on Investment” for the busy professional.
1. Selective Tissue Targeting
2. Micrometric Precision
Traditional bone fractures can sometimes be unpredictable, leading to irregular edges or the need for more extensive healing. Ultrasonic tips allow the surgeon to “draw” or “polish” the bone with the precision of a master jeweler. This level of accuracy ensures that the nasal bridge is perfectly smooth from day one, reducing the need for the body to undergo the prolonged inflammatory response required to heal more traumatic bone injuries.
3. Structural Stability
By avoiding the blunt-force trauma of the mallet, the structural supports of the nose remain more stable. This enhanced stability allows for more predictable healing and reduces the likelihood of minor shifts during the recovery phase. A stable structure heals more efficiently, allowing the patient to feel physically “back to normal” much sooner than with traditional methods.
The “Rapid ROI” Protocol
The elite medical sector in Riyadh has integrated these technological advancements into a comprehensive “Executive Path” designed for those with no time to waste. As we move through 2026, the journey is characterized by “Ghost Protocols” that ensure absolute privacy and accelerated healing.
-
AI-Enhanced Planning: Before surgery, 3D morphing and AI diagnostics allow the surgeon to map the procedure with absolute certainty. This “measure twice, cut once” approach ensures that the surgery is as efficient as possible, reducing time spent under anesthesia.
-
Regenerative Aftercare: Modern clinics now utilize advanced recovery aids, such as hyperbaric oxygen therapy and personalized lymphatic drainage, to flush out residual swelling. When combined with the gentle nature of Piezo surgery, these protocols can have an individual looking “Event-Ready” in a fraction of the traditional time.
-
Virtual Follow-ups: Recognizing the global nature of their patients’ lives, Riyadh’s top specialists offer secure, digital concierge follow-ups, allowing the executive to continue their travels or work while staying under the watchful eye of their consultant.
Beyond the Mirror
A truly mastered profile is one that enhances performance as much as it enhances image. For the professional navigating the dry climate of the Najd, respiratory efficiency is a vital component of total wellness. Many leaders suffer from a deviated septum or narrow valves that impede airflow, leading to chronic fatigue and disrupted sleep—the enemies of a high-power career.
Ultrasonic technology allows for a more effective “Functional Rhinoplasty.” The surgeon can straighten the internal architecture with greater accuracy, optimizing breathing without the heavy trauma of traditional septoplasty. When oxygenation is improved, cognitive focus and physical stamina rise. This “Health ROI” is perhaps the most valuable benefit for a leader, providing them with the energy and clarity required to drive the Kingdom’s most ambitious projects forward.
Safety and the SFDA Gold Standard
Psychology of the Mastered Profile
The internal transformation that follows a successful, rapid refinement is profound. When a leader no longer feels the need to compensate for a feature they find out of balance. Their natural charisma and authority are fully unleashed. This surge in self-assuredness is a powerful tool in negotiations, public speaking, and high-level leadership. It is the moment where physical harmony meets psychological strength—the final piece of the “Architecture of Confidence.”
Conclusion
In a city that defines itself by visionary leadership and rapid transformation, your personal image should be an asset, not a distraction. Achieving facial balance through the precision of ultrasonic technology is a strategic decision. That respects both your heritage and your time. By choosing a path defined by medical innovation, artistic integrity, and absolute discretion, you can secure a profile. That is both timeless and commanding without sacrificing your professional momentum.
Whether you seek to optimize your respiratory health or refine your silhouette for the global stage. The definitive standard remains professional Ultrasonic Rhinoplasty in Riyadh. To begin your bespoke journey toward a more balanced and confident future, and to experience the pinnacle of luxury surgical care. Trust your profile to the world-class specialists at Aesthetic Clinic Riyadh.
Equipments
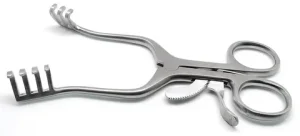
Cervical Self-Retaining Dull Retractor: Surgical Instrumentation
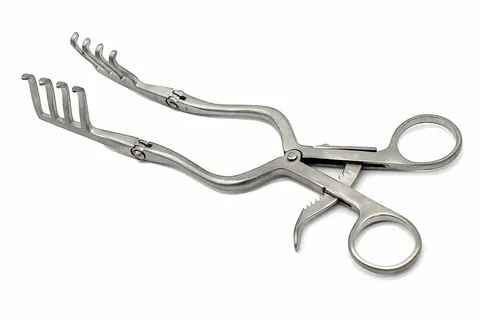
With decades of experience in the medical industry, we pride ourselves on delivering precision-crafted tools designed to meet the rigorous demands of surgeons, doctors, and medical professionals worldwide. In the complex arena of spinal procedures, having the right equipment is not just a matter of convenience; it is a critical factor that directly influences patient outcomes. Our specialized instrumentation line features the cervical self-retaining dull retractor, a masterpiece of biomedical engineering built to provide maximum exposure with minimal tissue disruption.
By combining robust mechanical design with highly specialized ergonomics, this tool allows surgical teams to maintain a clear, steady field of view throughout long and intricate operations without requiring constant manual adjustment.
Cervical Self-Retaining Dull Retractor
Navigating the delicate structural anatomy of the anterior and posterior neck requires an unmatched level of stabilization and control. The cervical self-retaining dull retractor addresses this challenge by incorporating a sophisticated, multi-position locking mechanism that holds the operative site open safely and independently. This self-locking capability frees up the assistant’s hands, allowing the entire surgical team to focus entirely on the delicate decompression or stabilization tasks at hand.
Because the mechanism spreads force evenly across its specialized arms, it minimizes the risk of sudden slippage or unexpected mechanical shifts during the procedure. This reliable mechanical stability is essential for maintaining the unyielding precision required when working in close proximity to critical neurovascular structures and the spinal cord.
Protecting Delicate Structures
One of the most defining characteristics of this premier surgical instrument is its focus on atraumatic tissue management. The cervical self-retaining dull retractor features precisely contoured, non-sharp blades designed specifically to pull back muscles, ligaments, and soft tissues without tearing or piercing them. Sharp retractors carry an inherent risk of causing micro-trauma or unintended punctures to surrounding vessels and nerves, which can lead to postoperative complications or extended healing times.
By utilizing a dull edge configuration, our device distributes retraction pressure smoothly across a wider surface area. This senn retractor thoughtful design drastically reduces the localized ischemic pressure on retracted muscles, preserving tissue integrity and significantly lowering the risk of post-surgical necrosis or chronic patient discomfort.
Workflow Efficiency in the Operating Room
Beyond structural safety, the physical architecture of our instrumentation line significantly enhances overall operating room workflow and surgeon comfort. The cervical self-retaining dull retractor is engineered with a streamlined, low-profile frame that maximizes the visible working workspace while remaining completely out of the way of primary surgical tools.
The ergonomic handles and responsive adjustment knobs ensure that changing the width or angle of retraction is smooth, predictable, and can be executed with minimal physical exertion. This intuitive operability is incredibly valuable during prolonged spinal fusions or multi-level disc replacements, where repetitive adjustments can introduce physical fatigue and slow down the momentum of the surgical team.
Strict Sterilization Standards
At Grey Medical, we understand that a surgical tool is only as reliable as the raw materials from which it is forged. Every cervical self-retaining dull retractor we manufacture is crafted from high-grade, medical-quality stainless steel that boasts exceptional tensile strength and superior resistance to environmental corrosion. This premium material selection guarantees that the instrument can withstand the punishing conditions of repeated high-temperature autoclaving and chemical sterilization cycles without losing its structural rigidity or joint fluidness.
By preventing material degradation and micro-pitting over time, our manufacturing process ensures that the retractor maintains a flawless, sterile surface, preventing pathogen buildup and safeguarding your patients against cross-contamination risks. Beyond structural safety, the physical architecture of our instrumentation line significantly enhances overall operating room workflow and surgeon comfort.
This intuitive operability is incredibly valuable during prolonged spinal fusions or multi-level disc replacements, where repetitive adjustments can introduce physical fatigue and slow down the momentum of the surgical team.
Clinical Excellence in Healthcare
Choosing the right surgical equipment is an investment in the long-term success of your medical practice and the safety of the patients who place their lives in your hands. The cervical self-retaining dull retractor exemplifies our ongoing commitment to pairing clinical functionality with manufacturing excellence. Medical institutions across the globe choose Grey Medical because our instruments consistently perform under pressure, day in and day out.
We continuously collaborate with leading neurosurgeons and orthopedic specialists to refine our designs, ensuring that every curve, lock, and finish aligns perfectly with the evolving standards of modern medicine. When you equip your operating room with our premium retractors, you are choosing a legacy of reliability, safety, and peerless surgical performance.
This premium material selection guarantees that the instrument can withstand the punishing conditions of repeated high-temperature autoclaving and chemical sterilization cycles without losing its structural rigidity or joint fluidness. By preventing material degradation and micro-pitting over time, our manufacturing process ensures that the retractor maintains a flawless, sterile surface, preventing pathogen buildup and safeguarding your patients against cross-contamination risks.
Beauty Fitness
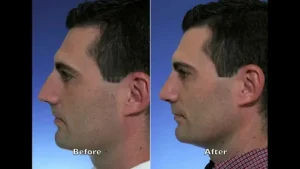
Male Rhinoplasty Specialists: Expert Nose Reshaping
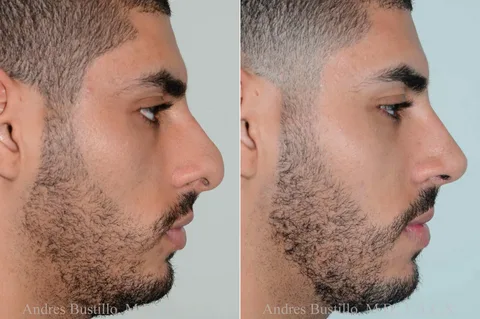
Male rhinoplasty specialists in Islamabad are experienced ENT and plastic surgeons who focus on male nose reshaping with natural, masculine results. Male rhinoplasty is different from female nose surgery because it aims to maintain a strong, straight, and balanced nasal profile rather than a delicate or overly refined shape.
What is Male Rhinoplasty?
It can help correct:
- Nose hump or dorsal bump
- Crooked or deviated nose
- Wide nasal bridge
- Drooping nose tip
- Breathing issues
- Trauma-related nasal deformities
Trusted Male Rhinoplasty Specialists in Islamabad
1. ENT & Rhinoplasty Experts
One of the most experienced specialists in Islamabad is Dr. Akhtar Zaman, an ENT surgeon with advanced expertise in male rhinoplasty, revision surgery, and functional nasal correction. He performs both cosmetic and medical nose procedures, making him a trusted option for men with breathing issues as well.
He is known for:
- Natural masculine nose shaping
- Septoplasty with rhinoplasty
- Functional breathing correction
- Revision rhinoplasty cases
2. Plastic & Cosmetic Surgeons
3. Specialized Rhinoplasty Clinics
Key Features of Male Rhinoplasty
Male rhinoplasty is designed to preserve masculine features, so surgeons focus on:
- Straight and strong nasal bridge
- Slightly defined but natural tip
- Balanced nose-to-face ratio
- Avoiding overly upturned or small nose shape
The goal is not to feminize the face but to improve structure while maintaining strength and character.
Modern Techniques Used in Islamabad
Male rhinoplasty specialists in Islamabad use advanced techniques such as:
- Open rhinoplasty (for detailed reshaping)
- Closed rhinoplasty (no visible scars)
- Ultrasonic rhinoplasty (less trauma, more precision)
- Sept rhinoplasty (for breathing + cosmetic improvement)
- Revision rhinoplasty (for correcting previous surgery)
These methods help ensure safer procedures and more predictable results.
Why Men Choose Rhinoplasty
Men choose rhinoplasty in Islamabad for several reasons:
- To improve facial confidence
- To correct long-term nasal deformities
- To fix breathing problems
- To enhance profile for professional appearance
- To repair injury-related nasal damage
Recovery After Male Rhinoplasty
Recovery is usually similar for men and women:
- Swelling and mild bruising for 1–2 weeks
- Return to routine work in 7–14 days
- Final results appear gradually over 3–6 months
- Full healing may take up to 1 year
Conclusion
Male rhinoplasty specialists in Islamabad focus on creating natural, masculine, and balanced nose shapes while also improving breathing function when needed. Experienced surgeons such as Dr. Akhtar Zaman and Dr. Hijrat, along with modern clinics like JJ Aesthetics, provide safe and customized rhinoplasty solutions using advanced surgical techniques. Choosing a skilled specialist ensures natural results, better facial harmony, and long-term satisfaction.
In addition to aesthetic enhancement, male rhinoplasty also plays an important role in correcting structural issues that may affect nasal airflow and overall health. Many patients seek surgery not only to improve appearance but also to resolve long-standing breathing difficulties caused by a deviated septum or trauma. Modern surgical planning in Islamabad involves detailed facial analysis, 3D imaging, and personalized treatment strategies to ensure results that suit each individual’s masculine facial proportions.
-
Business3 years ago
Cybersecurity Consulting Company SequelNet Provides Critical IT Support Services to Medical Billing Firm, Medical Optimum
-
Business3 years ago
Team Communication Software Transforms Operations at Finance Innovate
-
Business3 years ago
Project Management Tool Transforms Long Island Business
-
Business3 years ago
How Alleviate Poverty Utilized IPPBX’s All-in-One Solution to Transform Lives in New York City
-
health3 years ago
Breast Cancer: The Imperative Role of Mammograms in Screening and Early Detection
-
Sports3 years ago
Unstoppable Collaboration: D.C.’s Citi Open and Silicon Valley Classic Unite to Propel Women’s Tennis to New Heights
-
Art /Entertainment3 years ago
Embracing Renewal: Sizdabedar Celebrations Unite Iranians in New York’s Eisenhower Park
-
Finance3 years ago
The Benefits of Starting a Side Hustle for Financial Freedom