health
The Brave Little Fighters: Understanding the Unique Challenges of Childhood Cancer

Childhood cancer is a topic that touches the hearts of many. It’s difficult to think about innocent children facing such a challenging and life-altering illness. However, it’s important to understand the unique challenges that these brave little fighters face every day. From their treatment plans to their emotional well-being, childhood cancer presents its own set of obstacles that require attention and understanding. In this blog post, we’ll explore what makes childhood cancer so different from other illnesses, and how we can support these young warriors in their fight against cancer.
What is Childhood Cancer?
Childhood cancer is a type of cancer that affects children. It is the leading cause of death by disease in children under the age of 15. There are many types of childhood cancers, but the most common are leukemia, brain tumors, and lymphoma.
Childhood cancer is different from adult cancer in many ways. The biggest difference is that children’s bodies are still growing and developing, so the cancer can grow faster and spread to other parts of the body more easily. Children also have a higher risk of developing certain types of cancers, such as leukemia, than adults do.
Treatment for childhood cancer is also different from adult cancer treatment. Children’s bodies are more sensitive to the side effects of chemotherapy and radiation therapy, so these treatments are often given at lower doses. Surgery is also often used to treat childhood cancers, as it is less likely to cause long-term side effects than radiation or chemotherapy.
The survival rates for childhood cancer have improved dramatically over the past few decades. The overall five-year survival rate for all childhood cancers is now 80%, and it is even higher for specific types of cancers such as leukemia (89%) and brain tumors (94%). However, there is still much room for improvement, as many children with cancer still do not survive their disease.
The Different Types of Childhood Cancer
There are many different types of childhood cancer, each with its own set of unique challenges. The most common type of childhood cancer is leukemia, which accounts for about 30% of all cases. Other common types include brain tumors, lymphoma, and solid tumor cancers.
Each type of childhood cancer has its own set of symptoms and treatment options. Leukemia, for example, is typically treated with chemotherapy. Brain tumors may be treated with surgery, radiation therapy, or both. Lymphoma may be treated with radiation therapy or chemotherapy. And solid tumor cancers may be treated with surgery, radiation therapy, or a combination of both.
The prognosis for each type of childhood cancer varies depending on the specific diagnosis. In general, however, survival rates for all types of childhood cancer have been increasing in recent years thanks to advances in medical research and treatment options.
The Causes of Childhood Cancer
There are many different types of childhood cancers, and each has its own set of causes. In general, cancer is caused by the abnormal growth of cells in the body. This can happen as a result of a genetic mutation, exposure to certain environmental factors, or a combination of both.
Some specific causes of childhood cancer include:
• Exposure to ionizing radiation: This type of radiation is found in X-rays, CT scans, and other medical imaging procedures. It can also come from nuclear power plants and other sources. Studies have shown that children who are exposed to ionizing radiation are at an increased risk for developing leukemia and brain tumors.
• Chemicals: Children who are exposed to certain chemicals, such as benzene and pesticides, may be more likely to develop cancer.
• Infections: Some viruses and bacteria can increase the risk for developing certain types of childhood cancers, such as leukemia and lymphoma.
• Genetic mutations: Certain genetic mutations can be passed down from parents to children and increase the risk for developing cancer.
The Symptoms of Childhood Cancer
There are a number of different symptoms that can indicate childhood cancer. Some of the more common ones include:
– Persistent fevers that don’t respond to medication
– Unexplained weight loss or poor appetite
– Fatigue or lethargy
– Pain in the bones or joints
– Lumps or swellings anywhere on the body
– easy bruising or bleeding
– Recurrent infections
– Abnormalities with the eyes, such as redness, swelling, or discharge
The Treatment of Childhood Cancer
Though cancer in children is rare, accounting for less than 1% of all cancers diagnosed annually in the United States, it is the leading cause of death by disease in children under the age of 15.
There are many types of childhood cancer, and each requires its own unique treatment plan. In general, though, treatment will involve a combination of surgery, radiation therapy, and/or chemotherapy. The specific approach will be determined by the child’s age, overall health, and the type and stage of cancer.
Childhood cancer can be a very difficult thing for a family to deal with. Not only is it emotionally devastating to watch your child suffer, but it can also be financially ruinous. The good news is that there are many organizations dedicated to helping families dealing with childhood cancer. These organizations can provide financial assistance, emotional support, and practical help with day-to-day tasks.
The Unique Challenges of Childhood Cancer
Cancer is a scary diagnosis at any age, but it can be especially frightening for children. Not only are they faced with a potentially life-threatening illness, but they must also deal with the side effects of treatment, which can be both physically and emotionally challenging.
In addition to the physical challenges, childhood cancer can also take an emotional toll on patients and their families. The diagnosis can be overwhelming and scary, and treatment can be long and difficult. Children with cancer often miss out on important milestones like school graduation or prom, and they may feel isolated from their friends. Families may also struggle with the financial burden of treatment, as well as the emotional roller coaster of watching their child go through such a tough experience.
But despite all of these challenges, childhood cancer patients are brave little fighters. They show tremendous courage in the face of adversity, and they inspire us all to never give up hope.
Conclusion
Childhood cancer is a heartbreaking experience for families and communities alike. We must never forget the brave little fighters who courageously face this unique challenge every single day, and we must do all that we can to support them. With knowledge of the different types of childhood cancer, their risk factors, and the treatments available, we can start to take meaningful steps towards improving outcomes with these courageous children in our lives. Let’s stand together against childhood cancer and give these young warriors the strength they need to beat this horrible disease!
Beauty Fitness
Liposuction: Cheap vs Premium Clinics for Effective Results

Liposuction in Islamabad is becoming increasingly popular among people looking to achieve a slimmer body. With many clinics offering varying prices, it’s essential to understand the difference between cheap and premium options. Your choice can affect both the results and your safety.
Understanding Cheap Liposuction in Islamabad
Cheap Liposuction in Islamabad is often chosen by patients looking for affordable ways to remove stubborn fat. The lower cost can make the procedure appealing, especially for those on a tight budget. However, it’s important to understand what “cheap” really means in this context. Often, these procedures may use older equipment or be performed in clinics with less experienced staff.
While cheap Liposuction in Islamabad can deliver results, the quality of care and safety may not match premium clinics. There is a higher chance of complications such as uneven fat removal, infection, or longer recovery periods. Patients should carefully research the clinic, check surgeon qualifications, and read patient reviews before deciding.
Natural ways to prepare for surgery, such as maintaining a balanced diet and regular exercise, can improve outcomes regardless of the clinic you choose. Aftercare is equally important, but some budget clinics may not provide comprehensive guidance.
In short, cheap Liposuction in Islamabad can be an option for those mindful of costs, but safety and results should remain a priority. Investing time in research and preparation ensures you achieve better outcomes while minimizing risks.
Premium Liposuction in Islamabad
Premium Liposuction in Islamabad offers advanced technology and highly trained surgeons. Clinics offering premium services provide a safer environment and personalized care. The procedure usually results in smoother outcomes and faster recovery. While more expensive, the long-term benefits are often worth the investment.
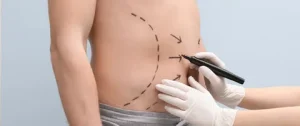
Key Differences Between Cheap and Premium Liposuction
Here are some major points to consider when choosing between cheap and premium Liposuction in Islamabad:
- Cost vs Safety: Cheap options save money but may compromise on safety.
- Experience of Surgeons: Premium clinics employ certified, experienced professionals.
- Equipment Quality: Advanced tools in premium clinics ensure better results.
- Aftercare Support: Premium clinics provide structured follow-up for recovery.
- Hospital Standards: Higher-end clinics follow strict hygiene and safety standards.
Why Cost Shouldn’t Be the Only Factor
While affordable Liposuction in Islamabad is tempting, focusing solely on cost can be risky. Quality of care, surgeon expertise, and clinic standards directly impact your results. Natural ways to prepare for surgery, like maintaining a healthy diet and exercise routine, can improve outcomes regardless of the clinic you choose.
Recovery and Aftercare
Recovery and aftercare are crucial steps following Liposuction in Islamabad to ensure safe healing and optimal results. After the procedure, patients may experience swelling, bruising, or mild discomfort. These are normal and usually subside within a few weeks. Following your surgeon’s instructions is essential to minimize complications and achieve the desired outcome.
Most premium clinics recommend wearing compression garments to support the treated areas. These garments help reduce swelling and contour the body shape. Pain management is also important, and your doctor may prescribe mild medications to ease discomfort. Regular check-ups during the first few weeks allow the surgeon to monitor healing progress.
Incorporating natural ways to enhance recovery can be very effective. Eating a balanced diet, staying hydrated, and engaging in light physical activity, such as short walks, can boost circulation and aid in faster healing. Avoiding smoking and alcohol is highly recommended as they can slow down the recovery process.
Proper aftercare also involves maintaining hygiene around the incision sites and promptly reporting any unusual symptoms to your surgeon. Choosing a reputable clinic ensures structured guidance, making your Liposuction in Islamabad experience safer and more satisfying.
Choosing the Right Clinic
Selecting the right clinic for Liposuction in Islamabad requires research. Look for reviews, surgeon credentials, and patient testimonials. Visiting the clinic before surgery helps you understand the environment and professionalism. Investing in a reputable clinic ensures your safety and satisfaction with the results.
FAQs About Liposuction in Islamabad
Q1: Is cheap liposuction safe?
A1: While possible, cheap Liposuction in Islamabad often carries higher risks due to older equipment or less experienced surgeons.
Q2: How long is the recovery time?
A2: Recovery usually takes 2–4 weeks, but premium clinics provide better guidance to speed up healing.
Q3: Can natural ways improve liposuction results?
A3: Yes, healthy diet, light exercise, and hydration help enhance results and reduce complications.
Q4: How do I choose between cheap and premium options?
A4: Evaluate clinic reputation, surgeon experience, equipment quality, and aftercare before deciding.
Q5: Are the results permanent?
A5: Liposuction in Islamabad provides long-lasting results if a stable lifestyle and natural ways of maintaining weight are followed.
Final Thoughts
Choosing between cheap and premium Liposuction in Islamabad is about balancing cost and safety. Prioritizing quality ensures better results, faster recovery, and minimal risk. For those seeking the best care and outcomes, trusted clinics like skn cosmetics offer professional services that meet international standards.
Care
Top Reasons Adults Choose Hormone Replacement Services in Houston
Hormone changes are a normal part of aging. As you get older, your body may not produce hormones at the same levels as before. These shifts can affect how you feel day-to-day, including your energy, sleep, mood, and focus. Many adults living in Houston begin to notice these changes and look for ways to better understand what is happening in their bodies.
Some people try to adjust their lifestyle first. They may improve their diet, exercise more, or work on sleep habits. While these steps are helpful, they do not always address hormone-related concerns fully. This is where structured evaluation and care can help.
Hormone-focused services look at your symptoms and lab test results to understand your body more fully. Instead of guessing, you receive information based on measurable data. This helps guide decisions and next steps in a clearer and more practical manner.
Key Reasons Adults Turn to Hormone Replacement in Houston Care
-
Addressing low energy that affects daily life
Many adults feel tired even after enough sleep, which can affect daily tasks and focus. Hormones such as thyroid hormone and testosterone help regulate energy levels. When these hormones are out of balance, you may feel drained without a clear reason.
Testing helps determine whether hormones are the cause, and care plans can then include hormone support, along with routine and nutrition guidance, to address the root issue rather than just the symptoms.
-
Supporting mood changes and mental clarity
Hormones influence brain function, including mood and concentration. When levels shift, you may notice irritability, stress, or difficulty staying focused.
These changes can affect your relationships, work, and overall quality of life. By reviewing hormone levels, a provider can look for patterns that may explain these symptoms. In some cases, adjusting hormone levels may help support more stable mood and clearer thinking.
This process is often combined with lifestyle habits such as regular sleep, balanced meals, and stress management techniques.
-
Managing natural hormone decline with age
Hormone levels change as part of the aging process. This happens in both men and women, although the patterns may differ.
For example, testosterone levels may decrease in men over time, while women may experience changes in estrogen and progesterone. These shifts can bring noticeable symptoms that develop slowly.
Regular evaluation helps track these changes over time. With ongoing monitoring, you and your provider can make informed decisions about whether support is needed and how to adjust care as your body changes.
-
Improving sleep quality and patterns
Sleep issues are often linked to hormone imbalance. Hormones such as cortisol and melatonin help regulate your sleep cycle.
If these hormones are out of balance, you may find it hard to fall asleep or stay asleep through the night. Poor sleep can then affect energy, mood, and overall health.
In cases where sleep problems are linked to hormones, evaluation can help identify the cause. Care may include hormone-related support, along with habits such as maintaining a consistent sleep schedule, limiting screen time before bed, and creating a calm sleep environment.
-
Supporting weight management efforts
Weight changes can be influenced by hormone levels. Hormones help regulate metabolism, appetite, and fat storage.
Some adults follow diet and exercise routines but still find it difficult to manage their weight. In these situations, hormone testing may provide more insight into what is happening inside the body.
A provider may review hormones related to metabolism, such as thyroid hormones and insulin. Based on the results, a plan may include a mix of hormone support, nutrition guidance, and physical activity recommendations.
-
Improving physical performance and recovery
Hormones also play a role in muscle strength, endurance, and recovery after exercise.
If your hormone levels are not balanced, you may notice reduced performance during workouts or longer recovery times. This can make it harder to stay consistent with fitness routines.
By checking hormone levels, providers can identify areas that may be affecting your physical performance. With proper guidance, you may see improvements in strength, stamina, and recovery when combined with regular exercise and proper rest.
-
Personalized care with ongoing monitoring
One main reason adults choose hormone-related services is the structured, personalized approach. Care is not a one-time visit. It usually includes consultation, lab testing, a tailored plan, follow-ups, and adjustments based on progress.
This step-by-step process helps track changes over time and ensures care is updated based on how your body responds. When considering options like hormone replacement in Houston, many adults prefer services that combine testing, guidance, and ongoing support for a clearer path forward.
Summary!
Hormone-related concerns can affect many areas of daily life, including energy, sleep, mood, weight, and physical performance. As these changes develop over time, it can be helpful to look at your health in a structured way that includes both testing and ongoing evaluation.
Choosing hormone-focused care allows you to better understand what is happening inside your body and take informed steps based on real data. With the right approach, you can work toward better balance while maintaining your daily routine and lifestyle.
In Houston, PUUR Health and Wellness offers a care model that focuses on personalized evaluation, monitoring, and guided support. This type of approach helps you move forward with clarity and consistent follow-up as part of your overall wellness plan.
Care
Ayurvedic Retinitis Pigmentosa Treatment: Holistic Eye Care

Living with retinitis pigmentosa (RP) can feel like an uphill battle. Everyday tasks that once seemed simple slowly become more challenging. You might struggle to see in dim light or notice that your peripheral vision is narrowing. These changes often create a significant amount of stress and anxiety. It is perfectly natural to feel overwhelmed when you are unsure about what the future holds for your sight.
In the United States, many people with RP are searching for ways to manage their condition beyond standard clinical care. While modern medicine excels at tracking the progression of the disease, it does not always provide long-term solutions to slow it down. This gap in care is why Ayurveda is gaining so much attention as a supportive option.
Ayurveda focuses on creating balance within your body and your daily habits. Instead of looking for a “quick fix,” this ancient system emphasizes steady and consistent care. In this comprehensive guide, we will explore how Ayurvedic principles can fit into your life as you manage the complexities of RP.
Understanding Your Condition and Setting Realistic Goals
Before you begin any new health regimen, you must understand exactly what RP is. It is a genetic condition that affects the retina’s ability to respond to light. Because it is hereditary, its effects vary wildly from person to person. Some individuals experience a very slow decline over decades. Others may see faster changes in their visual field.
Ayurveda encourages you to set realistic expectations from the start. You should not view this as an instant cure. Instead, you are working toward sustainable goals. These include maintaining your current level of vision, reducing daily ocular discomfort, and supporting the long-term health of your eye tissues. When you adopt this mindset, staying consistent with your care plan becomes much easier. It also helps lower your anxiety because you are focusing on what you can control today.

Supporting Your Body as a Complete System
Ayurveda does not view your eyes as isolated organs. Instead, it connects your vision to the overall balance of your entire body. According to this philosophy, your eyes depend on healthy digestion, efficient circulation, and strong nerve function. If one part of the system falters, the eyes feel the impact.
This is why an Ayurvedic approach to retinitis pigmentosa treatment often includes:
-
Herbal Supplements: These formulas support specific bodily functions like blood flow and cellular repair.
-
Gentle Detoxification: This process removes metabolic waste that might hinder your systemic health.
-
Customized Diet Plans: A specialized diet helps improve your “digestive fire,” ensuring your eyes get the nutrients they need.
Many people in the U.S. are now exploring this holistic approach. They appreciate that it looks at long-term wellness rather than just masking symptoms. By helping your body function better as a whole, you provide your eyes with a much stronger foundation for health.
Using Targeted Ayurvedic Eye Therapies
Ayurveda also offers specific treatments that focus directly on the ocular area. You should always undergo these therapies under the supervision of a trained professional. These methods aim to nourish the delicate tissues of the eye and soothe the optic nerve.
One commonly used method is Netra Tarpana. In this therapy, a practitioner applies medicated ghee (clarified butter) around the eyes for a set period. This process deeply hydrates the area and helps reduce the strain of constant squinting. Other techniques include gentle herbal cleansing to remove surface irritants and external herbal poultices.
While these therapies cannot reverse the genetic coding of RP, they can significantly improve how your eyes feel on a daily basis. They help reduce dryness, itching, and redness. Consistency is the secret to success here. You might not see a change after one session, but a structured plan often yields noticeable results over several months.
Making Simple Lifestyle Changes for Maximum Impact
Your daily routine plays a massive role in how you manage a chronic condition like RP. Ayurveda places heavy importance on simple, grounding habits. These small steps may seem basic, but they create a cumulative effect on your well-being.
You can start by auditing your kitchen. Prioritize fresh, home-cooked meals over processed or packaged foods. Processed items often contain preservatives that can cause systemic inflammation. Additionally, try to sleep at the same time every night. A regular sleep schedule allows your body to enter a deep state of repair.
Furthermore, you should limit your screen time whenever possible. Blue light from phones and computers can strain already sensitive retinas. You can also incorporate light eye exercises and relaxation techniques. Simple breathing exercises and daily meditation help reduce cortisol levels. Lowering stress is vital because high stress can negatively impact your overall immune response and eye health.
Combining Ayurveda with Modern Eye Care
You do not have to choose between ancient wisdom and modern science. In fact, many people find the most success when they combine both. This “integrative” approach allows you to get the best of both worlds. You can use modern technology to monitor the physical changes in your retina while using Ayurveda to support your body naturally.
With this balanced combination, you can:
-
Track Progress: Continue regular check-ups with your ophthalmologist to monitor vision changes accurately.
-
Follow a Plan: Stick to a structured Ayurvedic routine to keep your internal systems balanced.
-
Adjust as Needed: Work with both your doctor and your Ayurvedic practitioner to tweak your treatments based on your actual progress.
This proactive stance helps you feel more in control of your health. It moves you from a passive observer of your condition to an active participant in your care.
Conclusion: A Path Toward Consistent Care
Living with retinitis pigmentosa can certainly feel overwhelming at times. However, having a structured and compassionate approach can make a world of difference. Ayurveda offers a unique way to support your body through steady and intentional care. It prioritizes balance, routine, and long-term vitality over temporary results.
By understanding your condition deeply, making simple lifestyle adjustments, and exploring guided therapies, you can manage your daily life more effectively. Thousands of people are now adding Ayurveda to their care plans to improve their comfort and support their overall ocular health.
Organizations like the Netra Eye Institute are leading the way in this field. They provide structured programs that combine traditional Ayurvedic methods with a modern understanding of eye diseases. This type of comprehensive support helps you navigate the challenges of RP with more confidence and peace of mind. Remember, the goal is not to find a miracle but to build a lifestyle that protects and nourishes your vision for as long as possible. Starting today with small, consistent changes can lead to a much brighter future for your eye health.
-
Business3 years ago
Cybersecurity Consulting Company SequelNet Provides Critical IT Support Services to Medical Billing Firm, Medical Optimum
-
Business3 years ago
Team Communication Software Transforms Operations at Finance Innovate
-
Business3 years ago
Project Management Tool Transforms Long Island Business
-
Business3 years ago
How Alleviate Poverty Utilized IPPBX’s All-in-One Solution to Transform Lives in New York City
-
health3 years ago
Breast Cancer: The Imperative Role of Mammograms in Screening and Early Detection
-
Sports3 years ago
Unstoppable Collaboration: D.C.’s Citi Open and Silicon Valley Classic Unite to Propel Women’s Tennis to New Heights
-
Art /Entertainment3 years ago
Embracing Renewal: Sizdabedar Celebrations Unite Iranians in New York’s Eisenhower Park
-
Finance3 years ago
The Benefits of Starting a Side Hustle for Financial Freedom