health
How AI Technology is Shaping the Future of Healthcare
The Impact of AI on Healthcare
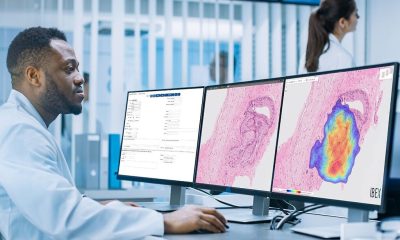
Artificial Intelligence (AI) is a game-changer in many fields, and healthcare is no exception. AI allows computers to analyze large amounts of information, identify patterns, and make recommendations. It’s like having a super-smart assistant that helps to solve complex problems. AI is used in many ways in healthcare, from preventive screenings to diagnosis and treatment. It’s like a virtual doctor that can help in many ways, without replacing the human touch.
The Benefits of AI in Healthcare
AI in healthcare can improve patient outcomes, reduce healthcare costs, and benefit overall population health. For instance, AI can speed up the process of cancer screenings, making results available faster. It can also help in assessing the risk of certain diseases. For instance, AI can identify people at risk of heart problems, even before they show any symptoms. This early detection can help in providing timely treatment and improving the patient’s quality of life.
AI and Machine Learning in Healthcare
AI and machine learning can help healthcare professionals in many ways. It can keep them up-to-date with the latest advances in medicine, take care of tedious tasks like writing clinical notes, and even help in making better decisions. However, it’s important to remember that AI is here to assist, not replace, healthcare professionals. They still play a crucial role in providing context, interpreting data, and communicating with patients.
Benefits:
- Artificial intelligence (AI) has revolutionized the way healthcare professionals manage chronic diseases such as asthma, diabetes, and high blood pressure. One of the most beneficial aspects of AI in this context is its ability to remind patients to take their medication on time and adhere to their care plan. For patients with asthma, AI can send notifications to remind them to use their inhaler or other prescribed medications at the appropriate times. This can help prevent asthma attacks and improve the overall management of the condition. Similarly, for individuals with diabetes, AI can provide reminders to check blood sugar levels, take insulin, and follow dietary recommendations. By promoting adherence to these essential tasks, AI can help prevent complications and maintain optimal health. In the case of high blood pressure, AI can monitor patients’ blood pressure readings and alert them if their levels are too high or too low. This proactive approach can lead to early detection of potential issues and prompt intervention to prevent serious consequences. Additionally, AI can track trends in blood pressure over time, providing valuable data that can guide treatment decisions and improve outcomes. Overall, AI has the potential to significantly enhance the management of chronic diseases by promoting medication adherence, monitoring key health metrics, and providing personalized support to patients. By leveraging the power of AI, healthcare providers can better support individuals living with chronic conditions and improve their overall quality of life..
- Artificial intelligence (AI) has revolutionized the way we can predict and respond to disease outbreaks. By analyzing social media posts and internet searches, AI can detect patterns and trends that may indicate the emergence of a disease in a particular region. This early warning system allows public health officials to take timely action to prevent the spread of diseases and mitigate the impact on communities. One of the key benefits of using AI for disease outbreak prediction is its ability to process vast amounts of data quickly and efficiently. By continuously monitoring social media posts and internet searches, AI can identify potential outbreaks before they become widespread. This proactive approach allows officials to implement targeted interventions, such as increased surveillance, vaccination campaigns, and public health messaging, to contain the spread of the disease. In addition to detecting outbreaks, AI can also help officials track the spread of diseases in real-time. By analyzing social media posts and internet searches, AI can provide valuable insights into how the disease is spreading and which populations are most at risk. This information allows officials to allocate resources more effectively and tailor their response strategies to the specific needs of the affected communities. Overall, AI has the potential to revolutionize the way we predict and respond to disease outbreaks. By harnessing the power of technology to analyze social media posts and internet searches, officials can take proactive measures to prevent the spread of diseases and protect the health and well-being of communities around the world.
- AI, or artificial intelligence, has the incredible potential to revolutionize the healthcare industry by significantly improving patient care. One of the ways in which AI can make a significant impact is through diagnosing diseases with a high level of accuracy. By processing and analyzing vast amounts of data, AI can quickly and efficiently identify patterns that might not be immediately apparent to human healthcare providers. This can lead to earlier detection of diseases and more timely interventions, ultimately improving patient outcomes. In addition to diagnosing diseases, AI can also play a key role in improving the quality of patient interactions. Through the use of natural language processing and machine learning algorithms, AI can provide empathetic responses to patient queries, ensuring that they receive the support and information they need in a timely manner. This can help to alleviate some of the stress and anxiety that patients may experience when seeking medical care, ultimately leading to a more positive overall healthcare experience. Overall, the integration of AI into healthcare has the potential to not only streamline processes and improve efficiency, but also to enhance the quality of care that patients receive. By leveraging the power of AI to accurately diagnose diseases and provide empathetic responses to patient queries, healthcare providers can deliver superior care that is both effective and compassionate.

Picture by: Yandex.com
Drawbacks:
- Without proper training, AI systems can unintentionally perpetuate bias and discrimination. This is why it is imperative to ensure that AI algorithms are trained on diverse data sets that accurately reflect the real-world population. By incorporating a wide range of perspectives and experiences into the training process, we can help mitigate the risk of AI systems making biased decisions that could harm marginalized groups. Diverse data sets allow AI systems to learn and adapt in a way that promotes fairness and equity. By exposing AI algorithms to a variety of inputs, including those from historically underrepresented communities, we can help prevent the perpetuation of harmful stereotypes and discriminatory practices. In doing so, we can create AI systems that not only perform effectively but also uphold ethical standards and promote social justice. In essence, the key to avoiding bias and discrimination in AI lies in the quality and diversity of the data used to train these systems. By prioritizing inclusivity and fairness in the training process, we can harness the power of AI to drive positive change and create a more equitable world for all.
- AI chatbots have been increasingly used in the healthcare industry to provide quick and convenient medical advice to patients. While these chatbots can be helpful in providing basic information and guidance, there have been instances where they have given misleading or false information, which can be detrimental to the patient’s health. In order to ensure the accuracy and safety of AI chatbots in providing medical advice, it is crucial to have effective regulations in place. These regulations can include requirements for chatbots to undergo rigorous testing and validation processes to ensure their accuracy and reliability. Additionally, healthcare providers and organizations should closely monitor the performance of AI chatbots and intervene when necessary to correct any inaccuracies. Furthermore, regulatory bodies and government agencies should establish guidelines and standards for the use of AI chatbots in healthcare settings. These guidelines can outline best practices for implementing and using chatbots, as well as provide mechanisms for reporting and addressing concerns about misleading or false medical advice. Overall, it is essential to regulate the use of AI chatbots in healthcare to protect patients and ensure that they receive accurate and reliable medical advice. By implementing effective regulations, we can maximize the benefits of AI technology while minimizing the risks associated with its use in the healthcare industry.
Looking ahead, AI has the potential to revolutionize healthcare by diagnosing currently undetectable conditions, predicting disease risk years in advance, and creating new ways to treat and prevent diseases. However, it’s important to use AI responsibly and ethically to ensure it benefits everyone.
Beauty Fitness
Ear Reshaping Surgery in Dubai: Bat Ear Correction & Procedure

Prominent ears, which people often call “bat ears,” represent a common anatomical variation. In these cases, the ears sit at a wider angle from the head than average. While this condition does not affect hearing or physical health, the aesthetic impact can feel significant. Many cultures highly value facial symmetry, and protruding ears can disrupt that balance. Ear Reshaping Surgery in Dubai offers a definitive medical correction for this trait. Surgeons utilize advanced techniques to “pin” the ears back, creating a more recessed and natural-looking profile.
What is Ear Reshaping Surgery in Dubai for Protrusion?
Clinical protrusion occurs when the distance between the ear rim and the side of the head exceeds two centimeters. Usually, an underdeveloped antithetical fold (the inner rim) or an oversized concha bowl (the deep cup) causes this gap. Ear Reshaping Surgery in Dubai serves as the clinical process for reconstructing these specific landmarks.
The surgeon performs the procedure as an outpatient treatment. They focus on structurally repositioning the cartilage to reduce the “fan-like” appearance of the ears. In our clinical experience, correcting protrusion stands as one of the most straightforward yet transformative aesthetic surgeries available today. Patients typically report that the change feels subtle. Friends and family notice the patient looks “better,” but they rarely realize the patient underwent surgery.
How the Procedure Sets Back the Ears
The procedure functions by modifying the spring and shape of the auricular cartilage. The surgeon begins by making a discreet incision hidden in the crease behind the ear. Through this opening, they access the cartilage framework.
The surgeon then uses internal, permanent sutures to “bend” the ear backward. If they encounter particularly stiff cartilage, they may employ “cartilage scoring.” This technique involves creating microscopic abrasions that allow the tissue to take on a new shape without tension. By anchoring these sutures to the dense tissue covering the mastoid bone, the surgeon “sets back” the entire ear structure. This ensures that the results remain structurally sound. It also prevents the natural tendency of cartilage to “spring” back to its original position.
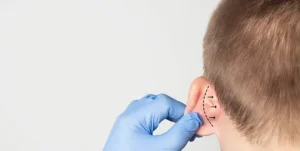
Why Choose Surgery for Prominent Ears?
The surgeon performs this intervention to bring the ears into a standard aesthetic range. Ideally, ears should sit at an angle of roughly 25 to 30 degrees from the head. Ear Reshaping Surgery in Dubai eliminates the “projection” that causes ears to stick out through hair or under hats.
This surgery serves as an essential tool for restoring facial balance. Ears that protrude too far can make the head appear wider or the face look asymmetrical. Beyond simple pinning, the surgeon uses the procedure to define the inner folds. Often, a “bat ear” looks flat and lacks detail. By recreating the antihelices fold, the surgeon gives the ear a more detailed, anatomically correct shape.
The Long-Term Benefits of Correction
Choosing to undergo surgery for protrusion offers several significant advantages:
-
Symmetrical Profile: The surgeon ensures both ears recessed to the same degree for a balanced look.
-
Natural Contour: Modern techniques avoid the “plastered to the head” appearance. Instead, they maintain a soft, natural curve.
-
Permanent Results: A single procedure provides a lifetime of correction.
-
Psychological Confidence: The surgery removes a frequent source of self-consciousness in social and professional life.
-
Hidden Scarring: The surgeon tucks all surgical marks away in the shadow behind the ear.
Identifying Ideal Candidates
The ideal candidate for Ear Reshaping Surgery in Dubai includes anyone over the age of five who feels bothered by their ear projection. For adults, the surgery finally addresses a trait they may have hidden for decades. For children, it represents a proactive step toward a more confident school experience.
During the consultation, the medical team evaluates the “spring” of your cartilage. They also measure the depth of your conchal bowl. This assessment helps them determine if a simple fold or a cartilage reduction offers the best path forward for your specific anatomy.
A Step-by-Step Look at the Pinning Process
The surgical journey follows a precise medical protocol to ensure safety and aesthetic accuracy.
-
Measurement: The surgeon uses calipers to mark the current projection and the target recessed position.
-
Incision: They make a vertical cut behind the ear where the tissue meets the scalp.
-
Cartilage Folding: The surgeon places permanent sutures to create or deepen the antihelical fold.
-
Conchal Setback: If the middle of the ear is too deep, the surgeon sutures it closer to the bone.
-
Final Verification: The surgeon checks the ears from the front to ensure the rim remains visible but no longer protrudes.
-
Bandaging: The team applies a compression wrap to protect the ears during the initial healing phase.
Common Treatment Areas and Corrective Zones
Surgeons focus on specific zones that contribute to the “bat ear” appearance.
| Protrusion Zone | Anatomical Focus | Surgical Correction |
| Superior Crura | The upper part of the ear rim. | Folds the top of the ear closer to the head. |
| Concha Bowl | The deep “cup” of the ear. | Reduces depth to pull the mid-ear inward. |
| Earlobe | The bottom fleshy part. | Ensures the lobe does not flare out. |
Cost Factors and Clinical Expertise
The investment in Ear Reshaping Surgery in Dubai reflects the intricacy of the ear’s cartilage. Stiff ears or those with multiple structural issues require more time and precision. When you choose a clinic with high standards, you pay for an expert who understands balance. They will not over-correct the ears. The true value lies in a result that looks natural and lasts a lifetime without the need for future revisions.
The Recovery Timeline
Patients typically report that the first week involves the most adjustment.
-
Days 1–3: You wear a bulky headband. Your ears may feel tight or throb slightly during this time.
-
Week 1: The surgeon removes the dressing. You can immediately see the new, closer position.
-
Weeks 2–6: You must wear a soft headband at night. This protects the internal sutures while you sleep.
-
Month 3: The ears fully “settle.” They will feel firm, natural, and permanent.
Safety and Long-Term Maintenance
The medical team maintains safety through sterile techniques and expert execution. Common side effects like temporary bruising or numbness resolve on their own. To maintain your new profile, you should follow these steps:
-
Sleep Carefully: Avoid side-sleeping for the first few weeks to prevent pressure on the sutures.
-
Handle with Care: Be gentle when putting on or taking off glasses or sunglasses.
-
Avoid Sports: Stay away from contact sports for 8 to 12 weeks. This allows the cartilage to harden fully in its new spot.
Conclusion: A More Balanced Future
Correcting “bat ears” provides a safe and effective way to bring balance to your facial features. It often brings a new level of confidence to your personal and professional life. Through the precision of Ear Reshaping Surgery in Dubai, you can achieve a profile that feels proportionate. Our team provides the medical excellence and care needed for a successful transformation.
Finance
Best Health Insurance Plan in India List Triggers Debate

The release of multiple lists claiming to identify the best health insurance plan in India has sparked widespread debate among consumers, insurers, and policy experts. This discussion has intensified as health insurance premiums have risen sharply by 25–50% across several policy categories. While insurers cite medical inflation, rising claim ratios, and advanced treatment costs as reasons, customers are questioning affordability, value for money, and long-term sustainability. At the center of this debate is whether a single list can truly define the best health insurance plan in India when individual needs, age, and medical history vary widely. The rising importance of add-ons such as critical illness insurance has further complicated how people evaluate health insurance plans today.
Why Health Insurance Premiums Are Rising Rapidly
One of the main reasons behind the premium hike is the steady rise in healthcare costs. Hospital charges, diagnostic tests, specialist consultations, and surgical procedures have become significantly more expensive over the last few years. Post-pandemic healthcare utilization has also increased, leading to higher claim volumes for insurers.
Another factor is the expansion of coverage. Modern policies now include mental health treatment, daycare procedures, and advanced therapies. While these benefits enhance coverage, they also increase costs. As insurers adjust pricing models to stay viable, customers are seeing steep premium hikes, even on policies previously considered the best health insurance plan in India.

Medical Inflation and Its Direct Impact on Policy Pricing
Medical inflation in India has consistently outpaced general inflation. Treatments that once cost a few lakhs now easily cross double-digit figures. This directly impacts insurers, who must reassess risk and pricing annually.
To balance rising payouts, insurers increase premiums across age brackets and policy renewals. Even long-term policyholders are not immune. This has led many consumers to question whether switching plans or reassessing what qualifies as the best health insurance plan in India is now necessary.
Debate Around Best Health Insurance Plan Lists
Lists ranking the best health insurance plan in India often rely on factors such as claim settlement ratios, network hospitals, premium cost, and coverage features. However, critics argue that such lists oversimplify a complex decision.
A plan suitable for a young professional may not work for a family with senior citizens. Similarly, a low-premium plan may exclude conditions that matter most to another individual. As premiums rise, the debate has shifted from which plan tops the list to which plan offers sustainable value over the long term.
Role of the Insurance Regulatory and Development Authority of India in Pricing Oversight
The insurance regulator plays a key role in ensuring transparency and fairness in premium pricing. While insurers are allowed to revise premiums based on actuarial data, they must justify hikes and follow regulatory guidelines.
The regulator also encourages standardization of policy wording and consumer awareness. This oversight helps customers make informed decisions while comparing options for the best health insurance plan in India, especially during periods of steep premium increases.
How Consumers Are Reacting to 25–50% Premium Hikes
For many households, a 25–50% premium hike has been a financial shock. Middle-income families, in particular, are reassessing their coverage amounts, deductibles, and add-ons.
Some consumers are opting for higher deductibles to lower premiums, while others are reducing sum insured levels. There is also growing interest in top-up and super top-up policies as cost-effective alternatives. These trends indicate that affordability is now as important as coverage when selecting the best health insurance plan in India.
Growing Importance of Critical Illness Insurance
As healthcare costs rise, critical illness insurance has gained renewed attention. Unlike regular health insurance, this cover provides a lump sum payout upon diagnosis of specified serious illnesses such as cancer, heart attack, or stroke.
With treatment costs for critical illnesses escalating rapidly, many policyholders are realizing that a standard health policy may not be enough. Adding critical illness insurance to an existing plan helps cover non-medical expenses such as income loss, travel, and long-term care, making it an essential consideration in today’s insurance planning.
Should Critical Illness Insurance Be a Separate Policy
One of the debates emerging alongside premium hikes is whether critical illness insurance should be purchased as a rider or as a standalone policy. Riders are often cheaper but may offer limited coverage. Standalone policies provide broader protection but come at a higher cost.
Given the rising premiums of base health policies, some consumers prefer standalone critical illness cover for focused protection. When evaluating the best health insurance plan in India, experts now recommend assessing how well it integrates with or complements critical illness insurance.
Impact on Families and Senior Citizens
Premium hikes have hit families with senior citizens the hardest. Older age groups already face higher premiums due to increased health risks. A sudden 30–50% hike can make renewals financially stressful.
This has sparked debates around affordability and inclusivity. Many argue that the best health insurance plan in India should balance comprehensive coverage with predictable long-term costs, especially for aging populations who need stability rather than frequent policy changes.
Are Insurers Offering Enough Value for Higher Premiums
Insurers defend premium hikes by pointing to expanded benefits, wider hospital networks, and improved claim processes. Some have introduced wellness programs, preventive health check-ups, and digital claim support to enhance value.
However, customers remain skeptical. Many feel that premium increases are not always matched by meaningful improvements in service. This perception gap has fueled discussions on whether the best health insurance plan in India should be judged by features alone or by real-world claim experiences.
How to Re-evaluate Your Health Insurance in the Current Scenario
With premiums rising, consumers are advised to review their policies carefully. Checking coverage limits, sub-limits, co-payment clauses, and waiting periods is essential.
Instead of switching policies frequently, experts suggest optimizing existing coverage by adding suitable riders or top-up plans. Aligning base health insurance with critical illness insurance can offer broader protection without drastically increasing costs.
Expert Opinions on the Premium Hike Debate
Industry experts believe that premium increases were inevitable given medical inflation and higher claims post-pandemic. However, they also stress the need for better communication from insurers.
Clear explanations of why premiums are rising and how customers benefit can help rebuild trust. Transparency is increasingly being seen as a key factor in defining the best health insurance plan in India.
Long-Term Outlook for Health Insurance in India
The current debate may lead to positive changes in the long run. Increased awareness is pushing consumers to understand policy details rather than relying solely on rankings or advertisements.
As demand for critical illness insurance grows, insurers are likely to innovate with flexible products and pricing models. This could eventually stabilize premiums while offering better value.
Conclusion
The debate triggered by lists of the best health insurance plans in India amid 25–50% premium hikes reflects a deeper shift in how Indians view health insurance. Rising costs have forced consumers to question affordability, coverage relevance, and long-term value.
While premium increases are driven by genuine factors such as medical inflation and higher claims, they have highlighted the need for smarter policy selection. Integrating base health coverage with critical illness insurance, reassessing personal needs, and focusing on sustainability rather than rankings can help consumers navigate this changing landscape more effectively.
Ultimately, the best health insurance plan in India is no longer defined by popularity or price alone, but by how well it protects individuals and families in an era of rising healthcare costs.
Care
Custom Fit Ear Plugs for Urban Noise Relief

Modern cities are full of energy, movement, and opportunity. However, they are also filled with constant noise. Traffic sounds, construction work, crowded public transport, and busy entertainment areas create environments that can be stressful for many people. Living in such places means that unwanted sound becomes a daily challenge. Many individuals are now turning to custom fit ear plugs as a practical way to manage noise and improve everyday comfort.
Urban noise is more than just an annoyance. It can affect sleep, concentration, productivity, and overall well-being. Whether someone is working, travelling, relaxing at home, or attending events, excessive noise may create discomfort and reduce quality of life. Custom ear protection offers a simple and effective solution to this growing problem.
This article explains how custom made ear plugs help people living in busy cities enjoy greater comfort, better focus, and improved hearing protection.
Understanding the Problem of Urban Noise
Cities are designed to support large populations, which means they are constantly active. While this activity supports economic growth and social life, it also creates a high level of noise exposure.
Common sources of urban noise include:
- Traffic congestion and vehicle horns
- Construction and building equipment
- Public transport systems
- Crowded entertainment venues
- Loud neighbors or nearby businesses
When people are exposed to these sounds every day, it may lead to stress, fatigue, and difficulty concentrating. Long-term exposure to loud environments can even affect hearing health.
Because avoiding city noise completely is almost impossible, many people look for solutions that help reduce sound without interrupting daily life.

What are custom-made earplugs?
Custom-made earplugs are hearing protection devices designed specifically for an individual’s ear shape. Specialists create them using a detailed ear impression so the final product fits comfortably and securely.
Unlike standard foam ear plugs that come in generic sizes, custom ear plugs provide:
- A precise and secure fit
- Better sound reduction
- Comfortable long-term use
- Durable and reusable materials
Businesses such as Earmold Sydney, an Australia-based provider with extensive experience and more than 100 satisfied customers, specialize in creating high-quality custom ear protection. Their personalized solutions help people manage noise in different environments.
Because the plugs are designed for the user’s ear canal, they remain comfortable even during long periods of use.
Improving Daily Comfort at Home
Many people expect their homes to be peaceful spaces where they can relax. Unfortunately, city living often includes unwanted noise from nearby streets, neighbors, or late-night activities.
Custom earplugs help create a quieter environment without requiring major lifestyle changes. By reducing outside noise, individuals can enjoy more relaxing moments at home.
Whether someone is reading, watching television, or simply resting after work, earplugs provide a calm atmosphere that supports mental well-being.
Better Sleep in Busy Cities
One of the most common problems in urban areas is poor sleep caused by noise. Traffic sounds, late-night entertainment, and early morning activity can interrupt sleep patterns.
High-quality sleeping earplugs help reduce these disturbances and create a quieter sleeping environment. When noise levels decrease, the body can relax more easily and fall into deeper sleep.
Better sleep improves mood, energy levels, and overall health. People who sleep well are often more productive and focused during the day.
For city residents, using earplugs at night can make a significant difference in daily comfort.
Support for Commuting and Travel
Public transport systems are an essential part of city life. However, trains, buses, and subways can be noisy and crowded.
Many commuters use custom ear plugs during travel to reduce environmental noise and create a more comfortable journey. Lower sound levels allow people to read, listen to music at safe volumes, or simply relax during their commute.
Reducing noise during travel also helps prevent hearing fatigue caused by continuous exposure to loud environments.
Protection for Motorcyclists
Motorcycle riders in busy cities face strong wind noise and traffic sounds while travelling at high speeds. Over time, this exposure can affect hearing health.
Specialized custom molded motorcycle ear plugs are designed to reduce wind noise while still allowing riders to hear important road sounds. This balance improves safety and comfort during long rides.
For urban riders who commute daily, proper ear protection helps prevent hearing damage and reduces fatigue caused by constant wind noise.
Enjoying Music Events Safely
Cities often host concerts, festivals, and entertainment events where sound levels can become extremely loud. While these experiences are enjoyable, they can also expose ears to harmful sound levels.
Many music lovers use earplugs for musicians because they reduce volume without completely blocking sound clarity. This allows individuals to enjoy music while protecting their hearing.
For people who attend concerts frequently, ear plugs provide a safe way to enjoy live performances without risking long-term hearing problems.
Protection During Swimming Activities
Swimming pools, beaches, and water sports facilities are common features of city life. However, water entering the ear canal can cause discomfort and infections.
Specialized designs considered the best earplugs for swimming help prevent water from entering the ear while maintaining comfort. These ear plugs create a secure seal that keeps the ears dry during swimming activities.
City residents who swim regularly benefit from this protection, especially when spending long periods in pools or open water.
Helping Professionals Stay Focused
Urban professionals often work in busy environments such as open offices, shared workspaces, or noisy neighborhoods. Background noise can reduce concentration and productivity.
Custom ear plugs help create a quieter working environment by reducing surrounding sound. This allows individuals to focus better on tasks, meetings, and creative work.
For business owners and professionals who rely on concentration, noise control becomes an important factor in maintaining productivity.
Long-Term Hearing Protection
Continuous exposure to loud environments may gradually damage hearing. Many people do not notice this damage until it becomes more serious.
Using custom ear plugs regularly helps reduce harmful noise levels and protect hearing health over time. Because they are comfortable, users are more likely to wear them consistently.
Preventing hearing damage early helps ensure long-term ear health and a better quality of life.
Durable and Reliable Protection
Custom ear plugs are made from high-quality materials such as silicone or acrylic. These materials are durable and easy to clean.
Unlike disposable earplugs, custom options can last for several years when properly maintained. This makes them a cost-effective solution for people living in noisy environments.
Reusable protection also reduces waste and provides consistent performance.
Why Choose Professional Ear Protection
Store-bought earplugs often fail to provide consistent results because they are not designed for individual ear shapes. They may feel uncomfortable or fall out during use.
Professional providers like Earmold Sydney specialize in personalized hearing protection solutions. With years of experience and over 100 happy customers across Australia, they focus on delivering reliable and comfortable ear plugs designed for real-life situations.
Their expertise ensures that each product fits perfectly and performs effectively in different environments.
Final Thoughts
City life brings many advantages, including access to work opportunities, entertainment, and social activities. However, constant noise can reduce comfort and affect well-being.
Custom-made earplugs provide a simple yet powerful solution for managing urban noise. They help people sleep better, focus at work, enjoy events safely, and protect their hearing during daily activities.
Whether commuting through busy streets, attending concerts, riding motorcycles, or relaxing at home, personalized ear protection improves everyday comfort.
With expert solutions from experienced providers such as Earmold Sydney, individuals living in loud cities can enjoy a quieter, healthier lifestyle while protecting their hearing for the future.
-
Business3 years ago
Cybersecurity Consulting Company SequelNet Provides Critical IT Support Services to Medical Billing Firm, Medical Optimum
-
Business3 years ago
Team Communication Software Transforms Operations at Finance Innovate
-
Business3 years ago
Project Management Tool Transforms Long Island Business
-
Business3 years ago
How Alleviate Poverty Utilized IPPBX’s All-in-One Solution to Transform Lives in New York City
-
health3 years ago
Breast Cancer: The Imperative Role of Mammograms in Screening and Early Detection
-
Sports3 years ago
Unstoppable Collaboration: D.C.’s Citi Open and Silicon Valley Classic Unite to Propel Women’s Tennis to New Heights
-
Art /Entertainment3 years ago
Embracing Renewal: Sizdabedar Celebrations Unite Iranians in New York’s Eisenhower Park
-
Finance3 years ago
The Benefits of Starting a Side Hustle for Financial Freedom