health
Blood Donation Guidelines for Gay and Bisexual Men
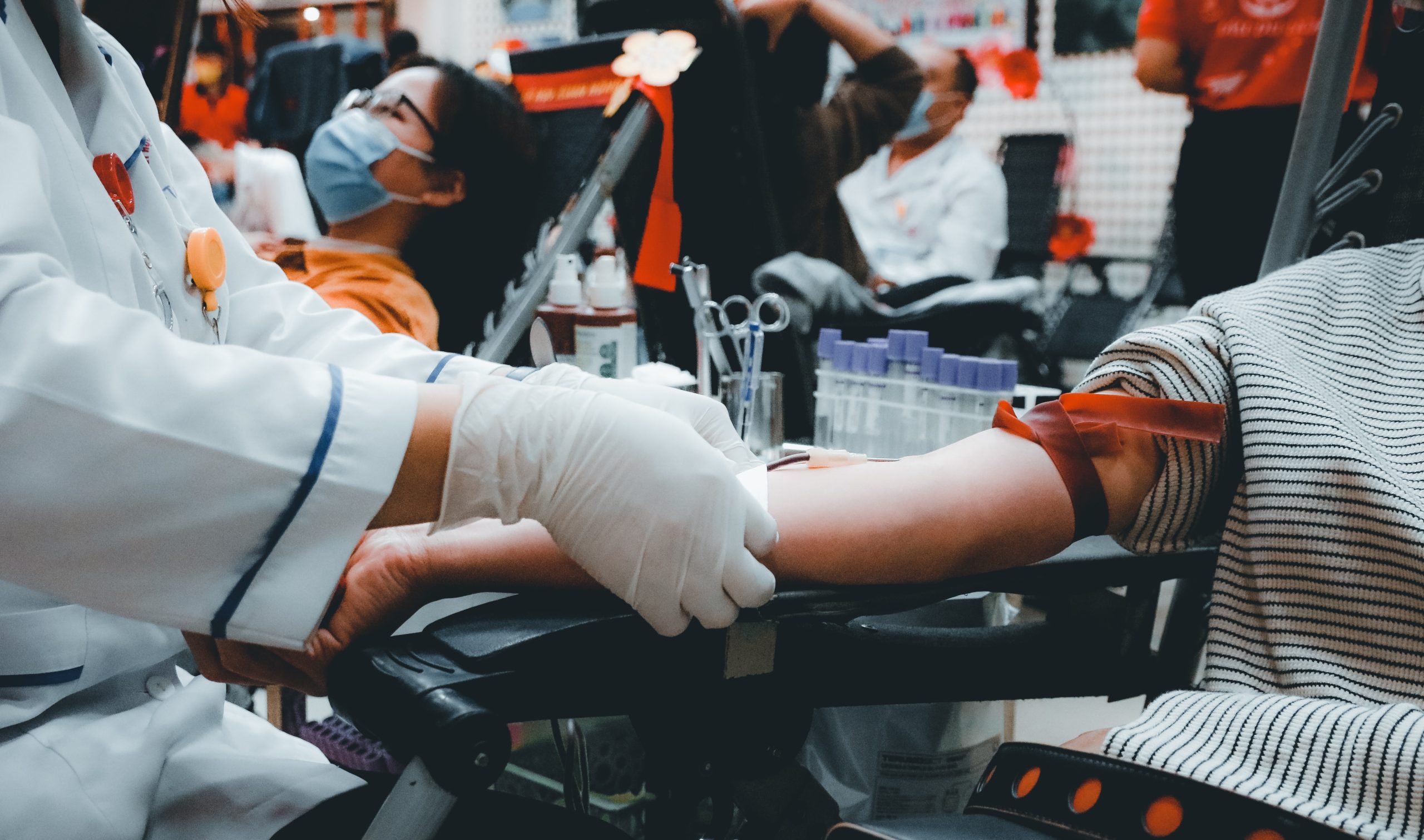
The U.S. Food and Drug Administration (FDA) has recently revised its blood donation guidelines for gay and bisexual men, reducing the required period of sexual abstinence from 12 months to three months. The decision represents a significant step forward in the fight for equality and inclusivity in the U.S. healthcare system.
The previous policy, which had been in place since the 1980s, completely banned blood donations from gay and bisexual men due to concerns over HIV transmission. In 2015, the FDA revised the ban to a 12-month deferral period, which required men who had sex with other men to wait a year after their last sexual encounter before donating blood. However, many advocates argued that the policy was still discriminatory and not based on scientific evidence.
The FDA’s latest decision to shorten the deferral period to three months comes after a thorough review of scientific research and data on HIV transmission and blood screening methods. According to the agency, recent studies have shown that the risk of transmitting HIV through blood transfusions is extremely low, even among donors who have recently engaged in sexual activity.
The change in policy has been widely welcomed by LGBTQ+ advocates and health experts. Many have long argued that the previous policy was based on outdated stereotypes and stigma, rather than scientific evidence. The new guidelines are seen as a significant step forward in the fight for greater inclusivity and equality in the healthcare system.
“This change reflects the best available scientific evidence and will help ensure more people are able to contribute to our nation’s blood supply while still protecting its safety,” said Peter Marks, director of the FDA’s Center for Biologics Evaluation and Research, in a statement.
The new guidelines also come at a critical time for the blood donation system. The COVID-19 pandemic has severely impacted blood donation rates, leading to shortages across the country. The FDA’s decision to revise the policy for gay and bisexual men could help increase the number of eligible donors and alleviate the strain on the blood supply.
However, some advocates argue that the new policy still falls short of true equality and inclusivity. The three-month deferral period is still based on assumptions about the sexual behaviors and practices of gay and bisexual men, rather than individual risk assessments. Critics also point out that other groups who may be at risk for HIV, such as heterosexual individuals who engage in high-risk sexual behaviors or intravenous drug users, are not subject to the same deferral periods.
In an opinion piece for The Advocate, writer Alex Bollinger argued that the new policy was a “step in the right direction,” but called on the FDA to adopt a risk-based policy that applies to all potential blood donors, regardless of sexual orientation or gender identity.
“The FDA’s latest move is a good one, but it doesn’t go far enough,” wrote Bollinger. “It’s time for the FDA to ditch outdated and discriminatory policies and adopt a risk-based policy that truly reflects the science and the realities of HIV transmission today.”
Despite these criticisms, the FDA’s decision to revise its blood donation guidelines for gay and bisexual men is a significant step towards greater equality and inclus.
Dental Health
Orthodontic Treatment Time: Average Duration & Factors

Orthodontic treatment is a highly effective way to improve tooth alignment, bite balance and overall oral health. One of the first questions patients ask before starting treatment is how long the process will take. While it would be reassuring to have a fixed answer, orthodontic timelines vary significantly from person to person. Treatment duration depends on individual dental needs, growth patterns and the type of appliance used.
Understanding how orthodontic treatment works, what influences its length and what to expect at each stage helps patients feel informed and confident. With realistic expectations and the right professional guidance, the orthodontic journey becomes far more manageable and rewarding.
What Is the Average Length of Orthodontic Treatment?
On average, orthodontic treatment lasts between 18 and 24 months. This timeframe applies to many common cases involving moderate crowding or bite issues. However, some patients may complete treatment in as little as 12 months, while others may require closer to 30 months or more.
The concept of an “average” simply reflects a broad range of cases. Teeth need time to move safely through bone, and the surrounding tissues must adapt gradually. Rushing treatment can increase the risk of discomfort, instability or relapse. This is why orthodontic care focuses on long-term success rather than speed alone.
Key Factors That Affect Orthodontic Treatment Time
Several important factors influence how long orthodontic treatment usually takes. These variables are assessed during the initial consultation and reviewed throughout treatment.
Key factors include:
- Severity of tooth misalignment or bite problems
- Jaw growth and skeletal relationships
- Age at the start of treatment
- Type of orthodontic appliance selected
- Patient compliance with instructions
For example, mild spacing may require minimal correction, while complex bite discrepancies involving jaw imbalance often take longer. In some cases, patients first seek care due to pain or appliance damage, sometimes visiting an emergency dentist in Durham, where underlying alignment issues are identified before orthodontic referral.
Treatment Duration by Orthodontic Appliance
Different orthodontic appliances are designed to address different types of dental issues, and this can affect treatment length.
| Appliance Type | Typical Treatment Time |
| Metal braces | 18–24 months |
| Ceramic braces | 18–24 months |
| Clear aligners | 12–24 months |
| Functional appliances | Varies by growth stage |
Clear aligners may offer shorter treatment times for mild to moderate cases when worn as directed. Fixed braces are often used for more complex movements that require precise control. An orthodontist Durham will recommend the most suitable appliance based on effectiveness rather than speed.
Does Age Impact Orthodontic Treatment Length?
Orthodontic treatment can be successful at any age, but biological factors may influence how efficiently teeth move.
- Children: Early orthodontic care may focus on guiding jaw growth rather than moving teeth extensively. Treatment may be shorter or delivered in phases.
- Teenagers: Teenagers often respond well to treatment because jaw growth is still ongoing. Many complete treatment within the average time range.
- Adults: Adult treatment can take slightly longer as the jawbone is fully developed. However, modern orthodontic techniques ensure predictable and stable results.
Regardless of age, good planning and compliance play a greater role in treatment duration than age alone.
The Role of Patient Compliance
Patient cooperation is one of the most significant factors affecting orthodontic treatment time. Even the best treatment plan relies on consistent effort from the patient.
Important compliance factors include:
- Wearing aligners for the recommended number of hours
- Attending appointments as scheduled
- Maintaining excellent oral hygiene
- Avoiding foods that damage braces
Missed appointments or repeated appliance breakages can slow progress considerably. In some situations, ongoing appliance issues may require visits to an emergency dentist in Durham, temporarily interrupting orthodontic progress and extending treatment duration.
Why Orthodontic Treatment Sometimes Takes Longer Than Expected
Delays in orthodontic treatment are not uncommon and are usually caused by avoidable factors. Understanding these helps patients stay on track.
Common reasons for extended treatment include:
- Poor aligner wear compliance
- Frequent bracket or wire breakages
- Missed or postponed appointments
- Gum inflammation or tooth decay
When dental health issues arise during treatment, orthodontic adjustments may pause until problems are resolved. This highlights the importance of oral hygiene and early professional advice when concerns appear.
Can Orthodontic Treatment Be Completed Faster?
Advances in orthodontic technology have improved efficiency and predictability, but safety and stability remain priorities. Accelerated treatment options may be appropriate for some patients, but they are not suitable for everyone.
Modern advancements include:
- Digital treatment planning
- Customised brackets and wires
- Improved aligner materials
These tools can streamline treatment, but rushing tooth movement can compromise results. Any decision to shorten treatment should be guided by an experienced orthodontist Durham, ensuring long-term stability is not sacrificed for speed.
Understanding the Stages of Orthodontic Treatment
Orthodontic treatment is delivered in stages, each contributing to the final result.
- Initial consultation and planning: Assessment, digital scans and treatment design.
- Active alignment phase: Gradual movement of teeth into healthier positions.
- Finishing and detailing: Fine adjustments to perfect alignment and bite.
- Retention phase: Use of retainers to maintain results long term.
Each stage is essential. Skipping or shortening phases increases the risk of relapse, even if teeth appear straight initially.
Setting Realistic Expectations
Orthodontic treatment is a gradual process, and progress may feel slow at times. However, noticeable changes often appear within the first few months, helping patients stay motivated.
Realistic expectations involve:
- Understanding that timelines vary
- Focusing on steady progress rather than speed
- Communicating openly with the orthodontic team
Patients who feel informed and supported are more likely to remain compliant and complete treatment on schedule.
Conclusion
There is no single answer to how much time orthodontic treatment usually takes, as every smile follows a unique path. While average treatment lasts around 18 to 24 months, factors such as case complexity, appliance choice and patient cooperation all influence the final timeline. What matters most is achieving safe, stable and lasting results rather than rushing the process. Orthodontic treatment is an investment in long-term comfort, confidence and oral health.
With personalized planning, modern techniques and professional support, patients can approach treatment with clarity and reassurance. With trusted orthodontic care available in Durham, individuals can move forward confidently, knowing their treatment timeline is carefully designed to deliver the best possible outcome for their smile.
health
Sports Medicine Detroit: Expert Care for Athletic Injuries

Sports and physical activity are essential for maintaining a healthy lifestyle, but they often come with the risk of injury. Whether you’re a competitive athlete, a gym enthusiast, or someone who enjoys weekend sports, injuries can disrupt your routine and impact your performance. That’s why many individuals seek care from specialists in sports medicine detroit, who are trained to diagnose, treat, and prevent sports-related injuries. With advancements in treatment methods and personalized recovery plans, athletes today can recover more efficiently and return to their activities with confidence and improved performance.
Understanding Common Sports Injuries in Detroit
Detroit has a strong and diverse sports culture, ranging from youth leagues and school athletics to adult recreational sports and fitness training. With such an active population, injuries involving muscles, joints, and ligaments are quite common.
Some of the most frequently treated sports injuries include:
-
Sprains and strains: These happen when ligaments or muscles are either stretched or torn, frequently as a result of abrupt movements or excessive effort
-
Knee injuries: ACL tears, meniscus damage, and patellar tendon issues are common, especially in high-impact sports.
-
Shoulder injuries: Repetitive motions in sports like baseball, swimming, or tennis can lead to rotator cuff injuries.
-
Tendonitis: Overuse injuries affecting tendons, often caused by repetitive stress without proper recovery.
-
Stress fractures: Small cracks in bones caused by repetitive force, common among runners and athletes in high-impact sports.
For example, consider a recreational weightlifter who experiences lower back pain after improper lifting technique. Ignoring the discomfort may lead to chronic issues, but early intervention through Back Pain Treatment can help address the problem effectively and prevent long-term complications.
Professionals in sports medicine detroit focus not only on identifying the injury but also on understanding how it occurred. This approach ensures that treatment plans address both symptoms and root causes.

How Sports Medicine Doctors Treat These Injuries
Modern sports medicine goes beyond simple rest and recovery. Today’s treatment strategies are comprehensive, combining medical care with rehabilitation and preventive techniques.
1. Accurate Diagnosis and Evaluation
The first step in treatment is a detailed assessment. Doctors perform physical examinations and may use imaging tools such as MRI or ultrasound to determine the severity of the injury.
2. Customized Treatment Plans
Each patient receives a personalized plan tailored to their specific condition, sport, and activity level. This ensures optimal recovery without unnecessary delays.
3. Rehabilitation and Physical Therapy
Rehabilitation is a key component of recovery. Programs focus on:
-
Restoring strength and flexibility
-
Improving joint stability
-
Enhancing range of motion
-
Preventing reinjury
4. Non-Surgical and Advanced Treatments
Many injuries can be treated without surgery using advanced techniques such as:
-
Targeted physical therapy
-
Anti-inflammatory treatments
-
Regenerative therapies
Studies suggest that structured rehabilitation programs can reduce reinjury rates by up to 50%, especially for ligament and muscle injuries.
Athletes who seek treatment through sports medicine detroit services often benefit from faster recovery times and improved long-term performance.
Expert Care and Patient-Centered Approach
Midway through recovery, having the right specialist guiding your treatment can make a significant difference. Clinics like Detroit Ortho Doc emphasize a patient-centered approach, ensuring that every individual receives care tailored to their needs.
Patients often consult Dr. Matthew J Yousif, DO, who specializes in diagnosing and treating sports-related injuries. His approach includes detailed evaluations, identifying movement patterns that may contribute to injury, and developing customized rehabilitation programs.
By focusing on both treatment and prevention, patients not only recover from their current injuries but also improve their overall physical performance. This comprehensive care helps athletes return to their activities with confidence while minimizing the risk of future injuries.
Real-World Applications and the Future of Sports Medicine Detroit
Sports medicine continues to evolve with advancements in technology and research, offering new ways to improve recovery and prevent injuries.
Some of the latest developments include:
-
Wearable technology: Devices that track movement patterns and detect early signs of injury
-
Biomechanical analysis: Advanced systems that evaluate how athletes move and identify inefficiencies
-
Regenerative medicine: Therapies that promote faster healing of tissues
-
Data-driven rehabilitation programs: Customized plans based on performance metrics
These innovations are transforming how sports injuries are treated and managed. For example, an athlete recovering from a knee injury may use wearable sensors to monitor movement during rehabilitation exercises, ensuring proper technique and reducing the risk of reinjury.
As these technologies become more accessible, Sports Medicine Detroit will continue to provide more effective and personalized care for athletes of all levels.
Frequently Asked Questions
What are the most common sports injuries treated by specialists?
Common injuries include sprains, strains, ligament tears, tendonitis, and stress fractures.
Can sports injuries heal without medical treatment?
Some minor injuries may heal with rest, but untreated injuries can worsen and lead to long-term complications.
How long does it take to recover from a sports injury?
When should I see a sports medicine doctor?
If you experience persistent pain, swelling, or reduced mobility for more than a few days, it’s important to seek medical evaluation.
Can sports medicine help prevent injuries?
Yes. Specialists provide guidance on training techniques, strengthening exercises, and recovery strategies to reduce injury risks.
Conclusion
Sports injuries are a common challenge for active individuals, but the right care can make a significant difference in recovery and long-term performance. Specialists in sports medicine detroit offer expert diagnosis, personalized treatment plans, and rehabilitation strategies that help patients recover safely and efficiently. By addressing injuries early and following structured recovery programs, athletes can return to their activities stronger and more confident. With continuous advancements in treatment and technology, sports medicine remains essential for maintaining an active and healthy lifestyle.
health
Laser Hair Removal in Dubai: Understanding the Science
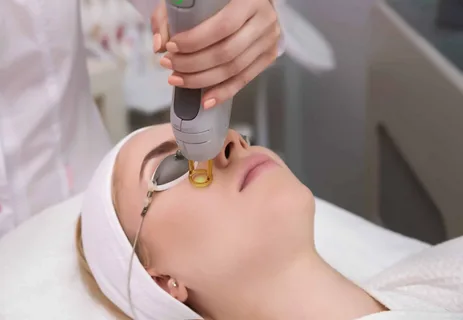
The shift from temporary grooming to permanent hair reduction is powered by one of the most precise applications of physics in modern aesthetics. While many focus on the visual results, the true value of Laser Hair Removal in Dubai lies in the complex interaction between light, heat, and human biology. By understanding the underlying science of how medical lasers operate, patients can better appreciate why multiple sessions are required and how technology ensures the safety of the surrounding skin.
Understanding the Science of Laser Hair Removal in Dubai
Laser technology has transformed the way we approach long-term hair reduction. At its core, this treatment relies on a scientific principle called selective photothermolysis. In simple terms, this means that a specific wavelength of light targets a specific structure without harming the surrounding skin.
In this procedure, the target is melanin, the pigment that gives hair its color. The laser uses a calibrated wavelength that melanin absorbs efficiently. As a result, the energy focuses directly on the hair follicle.
In our clinical experience, explaining this concept helps patients understand why results vary depending on hair color and skin type. Laser Hair Removal in Dubai works by delivering controlled heat to damage the hair follicle while protecting nearby tissue. Therefore, it is not just a cosmetic procedure but a medically guided treatment.
How Laser Hair Removal in Dubai Converts Light into Heat
When the practitioner places the laser handpiece on the skin, it emits a concentrated beam of light. This light passes through the outer skin layer and reaches the hair shaft. Since the hair contains more pigment than the surrounding skin, it absorbs the energy quickly.
As a result, the light energy transforms into heat almost instantly. This heat travels down the hair shaft and reaches two critical areas:
-
The bulb (hair root)
-
The bulge (growth center)
Once the temperature reaches the required level, it disrupts the follicle’s ability to regrow hair.
What patients typically report is a mild warming sensation during and after the session. This feeling reflects the controlled thermal process taking place within the follicle.
Why Laser Hair Removal in Dubai Requires Multiple Sessions
Many patients ask why several sessions are necessary. The answer lies in the natural hair growth cycle. Hair grows in three stages, and the laser only works effectively during one of them.
Hair growth phases include:
| Phase | Description | Laser Effectiveness |
|---|---|---|
| Anagen | Active growth phase | Highly effective |
| Catagen | Transition phase | Limited effect |
| Telogen | Resting phase | No effect |
Only about 15% to 20% of hair is in the active growth phase at any given time. Therefore, practitioners schedule sessions several weeks apart to target new hairs as they enter this stage.
In our clinical experience, patients who follow the recommended schedule achieve the most consistent and long-lasting results.
Benefits of Laser Hair Removal in Dubai Technology
Modern laser systems offer clear advantages over traditional methods like shaving or waxing. Because they rely on advanced physics, they provide more precise and long-term results.
Key benefits include:
-
Targeted treatment without damaging surrounding skin
-
Long-term hair reduction
-
Reduced ingrown hairs
-
Smooth skin texture
-
Faster treatment sessions with advanced devices
Additionally, modern lasers use a single wavelength, which allows focused energy delivery. This precision improves both safety and effectiveness.
Who Is the Ideal Candidate for Laser Treatment
Laser hair removal works best when there is a contrast between hair color and skin tone. Dark hair absorbs laser energy more effectively, making the treatment more efficient.
However, advanced technologies now allow safe treatment for a wider range of skin tones. For example, Nd:YAG lasers can treat deeper skin tones safely because they bypass surface pigment and target deeper follicles.
Ideal candidates include:
-
Individuals with dark or coarse hair
-
Patients seeking long-term hair reduction
-
Those tired of frequent shaving or waxing
On the other hand, very light, grey, or white hair may not respond well because it lacks sufficient pigment.
Step-by-Step Laser Hair Removal Procedure
A laser session follows a structured and controlled process. Each step ensures both safety and effectiveness.
Typical procedure includes:
-
Skin assessment and parameter selection
-
Adjustment of laser settings based on skin type
-
Application of cooling system for protection
-
Delivery of laser pulses in a grid pattern
-
Monitoring skin response during treatment
During the session, patients feel a light snapping or warming sensation. This indicates that the laser energy is reaching the follicle effectively.
Common Treatment Areas and Biological Differences
Different areas of the body respond differently due to variations in hair thickness and growth cycles.
| Area | Response to Treatment |
|---|---|
| Face | Faster cycles, more frequent sessions |
| Legs | Slower cycles, longer intervals |
| Underarms | Strong response due to coarse hair |
| Bikini | High effectiveness |
| Back/Chest | Requires deeper penetration |
Because of these variations, treatment plans are always customized.
Recovery and What to Expect After Treatment
Recovery after laser hair removal is simple and quick. Most patients return to normal activities immediately.
Typical recovery timeline:
First 24 hours
-
Mild redness or sensitivity
Days 2–3
-
Skin returns to normal
Days 10–14
-
Hair shedding occurs naturally
It is important to understand that shedding is part of the process, not new growth. The body gradually removes treated follicles over time.
Safety and Advanced Cooling Technology
Safety plays a critical role in laser treatments. Modern systems include built-in cooling mechanisms that protect the skin during the procedure.
For example, dynamic cooling devices release a cooling spray just before each laser pulse. As a result, the skin remains protected while the follicle absorbs the heat.
In our clinical experience, proper calibration and trained practitioners significantly reduce risks. Therefore, choosing a professional setting ensures both safety and optimal outcomes.
Maintaining Long-Term Results
After completing the initial sessions, most hair follicles remain permanently reduced. However, hormonal changes can sometimes stimulate new growth.
To maintain results, patients should:
-
Attend occasional maintenance sessions
-
Protect skin from excessive sun exposure
-
Follow pre- and post-treatment guidelines
Consistency plays a key role in preserving smooth, hair-free skin over time.
Conclusion
The science behind permanent hair reduction is a testament to the power of modern medical technology. By harnessing light and heat with clinical precision, we can offer results that were once considered impossible. At Tajmeels Clinic, we pride ourselves on our deep understanding of these scientific principles, ensuring that every pulse we deliver is safe, effective, and tailored to your biology. Learn if this treatment is right for your lifestyle by booking a consultation and discovering the science of smoothness for yourself.
-
Business3 years ago
Cybersecurity Consulting Company SequelNet Provides Critical IT Support Services to Medical Billing Firm, Medical Optimum
-
Business3 years ago
Team Communication Software Transforms Operations at Finance Innovate
-
Business3 years ago
Project Management Tool Transforms Long Island Business
-
Business3 years ago
How Alleviate Poverty Utilized IPPBX’s All-in-One Solution to Transform Lives in New York City
-
health3 years ago
Breast Cancer: The Imperative Role of Mammograms in Screening and Early Detection
-
Sports3 years ago
Unstoppable Collaboration: D.C.’s Citi Open and Silicon Valley Classic Unite to Propel Women’s Tennis to New Heights
-
Art /Entertainment3 years ago
Embracing Renewal: Sizdabedar Celebrations Unite Iranians in New York’s Eisenhower Park
-
Finance3 years ago
The Benefits of Starting a Side Hustle for Financial Freedom
































