health
From Opposition to Support: The Evolution of Medicaid Expansion in North Carolina

In the world of healthcare, Medicaid expansion has been a hotly debated topic for years. North Carolina was one of the states that initially opposed expanding its program, but after several years and changes in leadership, the state has now become an advocate. In this blog post, we will explore how North Carolina’s views on Medicaid expansion have evolved over time and what impact it has had on access to healthcare for thousands of residents in need. Get ready to dive into a story of political shifts, public opinion changes, and ultimately improved health outcomes!
Background: Medicaid Expansion in North Carolina
Since the Affordable Care Act (ACA) was implemented in 2014, Medicaid has been a popular topic of discussion among state policymakers. In 2013, North Carolina became one of 23 states to accept the ACA’s Medicaid expansion, which allows individuals with incomes below 138% of the federal poverty level (FPL) to qualify for coverage through the program.
The decision to expand Medicaid was met with fierce opposition from many conservative lawmakers and groups in North Carolina. However, after extensive research and deliberation, the State Board of Health decided that expanding Medicaid would be the best approach for addressing North Carolina’s high uninsurance rates. Since 2014, North Carolina’s uninsured rate has fallen from 17% to 8%, making it one of the fastest-growing states in terms of Medicaid enrollment.[1]
The decision to expand Medicaid has been overwhelmingly supported by North Carolinians. A statewide poll conducted by Public Policy Polling in late 2017 found that 66% of registered voters support expanding Medicaid under the ACA,[2] and a recent survey commissioned by UNC Health Care found that 81% of respondents believe that expanding Medicaid is important for improving healthcare access in North Carolina.[3]
The success story of North Carolina’s Medicaid expansion demonstrates the importance of bipartisan cooperation when implementing healthcare reform measures such as Obamacare. Despite strong opposition from some politicians and groups, expanded Medicaid has been an overwhelming success in reducing uninsurance rates and improving healthcare access for low-income residents across Southern states
The Opposition to Medicaid Expansion
The North Carolina Senate voted 50-43 on March 7, 2014 to expand Medicaid under the Affordable Care Act. This vote marked a major change from when the bill initially passed out of committee in January with only one dissenting vote (Sen. Phil Berger, R-Rockingham).
Initially, the majority of North Carolinians opposed Medicaid expansion because they believed it would be too costly for the state. However, after extensive research and hearings throughout the state, many legislators changed their minds and came to support the bill as it would provide healthcare coverage to low-income individuals who couldn’t afford it on their own.
Supporters of Medicaid expansion argue that without it, thousands of people will go without health care and will end up costing taxpayers more in emergency room visits and other medical expenses. Opponents of expansion point out that if the government is going to be providing health insurance benefits to able-bodied adults, then it should do so at no cost to taxpayers through Social Security instead of through Medicaid which is funded by general tax revenue.
The Development of Support for Medicaid Expansion
Since the Affordable Care Act (ACA) was enacted in 2010, there has been a notable shift in public opinion towards Medicaid expansion in North Carolina. In early 2011, nearly 60% of North Carolinians opposed Medicaid expansion, but as of June 2017 this figure had decreased to just 38%. This change is largely attributable to the work of advocacy groups who have been tirelessly working to convince North Carolinians that Medicaid expansion is a critical part of the ACA’s mission.
The key argument for expanding Medicaid is that it would provide coverage to more than 680,000 low-income adults in North Carolina. The vast majority of these beneficiaries are children, seniors, or people with disabilities who would not be able to afford coverage on their own. Improving access to health care for vulnerable populations is one of the most important benefits of expanding Medicaid eligibility.
Another argument for expanding Medicaid is that it would generate significant fiscal savings for the state. By 2022, expanded coverage under Medicaid would cost North Carolina less than $500 million per year – a negligible amount when compared to the state’s annual budget deficit.
Despite these compelling reasons, many North Carolinians continue to be resistant to extending coverage through Medicaid. Their concerns range from fear that government programs are inevitably wasteful and unsustainable to skepticism about whether individuals who are currently ineligible will actually become eligible under an expanded program. Notwithstanding these reservations, advocates remain optimistic that eventually enough North Carolinians will come around and support an expansion of
Conclusion
The North Carolina General Assembly passed HB488, the Medicaid Expansion and Work Requirements Act, on March 7th. This bill marks a significant change in North Carolina’s Medicaid history – from opposition to support. The path to passage wasn’t easy. The bill faced intense resistance from both doctors and patients alike, with protests and rallies taking place in every corner of the state. But through persistence and hard work, lawmakers were able to pass HB488 into law. And now that it is finally here, what does this mean for North Carolinians? HB488 changes how Medicaid works in North Carolina by instituting work requirements for recipients who are newly eligible for the program. This means that not only will people need to be able to find a job that pays at least 80 percent of their monthly income, but they will also need to participate in training or substance abuse treatment programs as part of their requirements. These are big changes, and they will impact millions of people across the state. But despite the challenges involved, lawmakers were able to pass HB488 because they believe it is important that North Carolinians have access to health care – no matter their income level or status in society.
Care
Mounjaro in Dubai: Every Stage of Your Treatment Journey
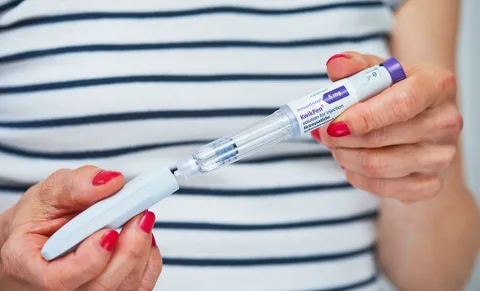
Embarking on a metabolic health journey requires patience, medical guidance, and realistic expectations. Over the last few years, Mounjaro in Dubai has become a trusted option for people managing type 2 diabetes and long-term weight concerns. Patients often feel more confident when they understand what happens at every stage of treatment. From the first consultation to long-term maintenance, each phase plays a key role in achieving safe and lasting results.
Initial Consultation and Assessment
Before treatment begins, doctors perform a detailed health evaluation. This process involves much more than simply prescribing medication. Specialists review blood sugar levels, kidney function, hormonal balance, and overall metabolic health to determine whether the treatment suits the patient.
During this stage, doctors also explain the titration process. Since the medication affects appetite hormones and insulin regulation, treatment starts with a low introductory dose. This gradual beginning helps the digestive system adapt safely while reducing the risk of discomfort.
In addition, patients receive guidance about hydration, meal planning, and healthy lifestyle habits. This preparation creates a stronger foundation for long-term success and improves treatment safety from the start.
Mounjaro in Dubai
The first month focuses mainly on adaptation. Most patients begin with a 2.5 mg weekly dose. Although this amount is considered introductory, many people quickly notice changes in appetite and eating behavior.
For example, patients often report fewer cravings and less emotional eating. Many also describe reduced “food noise,” which refers to constant thoughts about snacking or overeating. As digestion slows slightly, smaller meals start to feel more satisfying.
At the same time, mild side effects may appear. Some individuals experience nausea, bloating, constipation, or temporary fatigue. However, these symptoms usually improve as the body adjusts to the medication.
To support smoother adaptation, doctors commonly recommend:
- Drinking more water throughout the day
- Eating smaller portions slowly
- Prioritizing protein-rich meals
- Avoiding greasy or heavy late-night foods
- Staying physically active with light movement
Because the body is still adjusting hormonally, patience is important during these early weeks.
Active Fat Reduction Phase
This phase often produces the most visible physical changes. Appetite suppression becomes stronger, and the body begins using stored fat more efficiently for energy.
Mounjaro in Dubai and Dose Escalation
During weeks 5 to 8, many patients experience more consistent appetite control and noticeable waist reduction. Blood sugar readings also begin improving steadily for people with type 2 diabetes.
By weeks 9 to 16, weight loss patterns often become more stable. Patients frequently report:
- Better portion control
- Reduced cravings for sugary foods
- Increased energy levels
- Improved sleep quality
- More stable morning glucose readings
Furthermore, healthcare providers encourage resistance training and adequate protein intake during this period. These habits help preserve muscle mass while supporting healthy fat reduction.
Instead of focusing only on lower numbers on the scale, doctors emphasize body composition and metabolic improvement. This approach creates healthier and more sustainable outcomes over time.
Why Slow Titration Matters
Many patients wonder why doctors increase the dosage gradually rather than immediately using a higher amount. The answer lies in safety and long-term tolerance.
A structured titration schedule allows the digestive system and hormonal pathways to adapt step by step. As a result, patients are less likely to experience severe gastrointestinal side effects.
Additionally, slow dose escalation gives healthcare providers time to evaluate:
- Blood sugar response
- Digestive tolerance
- Hydration levels
- Energy patterns
- Overall metabolic improvement
If side effects become difficult at a certain level, doctors may keep the patient on the same dose for several extra weeks before increasing it again. This flexible strategy supports safer long-term success with Mounjaro in Dubai.
Benefits Beyond Weight Loss
Although many people begin treatment to lose weight, the long-term advantages extend far beyond appearance alone. Over time, patients often experience significant metabolic and cardiovascular improvements.
Some important long-term benefits include:
- Better HbA1c control
- Reduced visceral abdominal fat
- Improved cholesterol and triglyceride levels
- Better insulin sensitivity
- Lower inflammation markers
- More balanced hunger hormones
Moreover, many patients notice psychological improvements as their physical health improves. Increased mobility, better sleep, and improved confidence can positively affect emotional well-being and daily quality of life.
Because obesity and diabetes influence nearly every body system, consistent metabolic improvement often creates benefits that extend far beyond the scale.
Managing Side Effects Safely
Medical supervision remains extremely important throughout treatment. Although most side effects are mild, regular follow-up appointments help doctors monitor patient safety closely.
The most common side effects include:
- Nausea
- Acid reflux
- Constipation
- Mild stomach discomfort
- Reduced appetite
Fortunately, these symptoms usually decrease as the body adapts to each new dose level.
Doctors often help patients manage symptoms by recommending:
- Smaller meals throughout the day
- Slower eating habits
- Increased hydration
- Higher fiber intake
- Reduced fatty food consumption
Regular monitoring also helps protect kidney function, digestive health, and gallbladder health during treatment.
Expected Weight Loss Timeline
Every patient responds differently based on genetics, lifestyle, hormone balance, and medical history. However, clinical experience provides a general timeline for expected progress.
| Timeframe | Typical Dose | Common Progress |
|---|---|---|
| Month 1 | 2.5 mg | Early appetite suppression and mild fluid reduction |
| Months 2–4 | 5 mg to 10 mg | Steady fat reduction and improved glucose stability |
| Month 6+ | 12.5 mg to 15 mg | Greater waist reduction and stronger metabolic improvement |
Most patients lose weight gradually rather than instantly. In many cases, losing weight slowly leads to healthier and more sustainable long-term results.
Lifestyle Habits Still Matter
Although the medication is powerful, lifestyle habits continue to play a major role in success. Patients who combine treatment with healthier daily routines often achieve the strongest and most stable outcomes.
Doctors usually encourage:
- Whole-food nutrition
- Higher protein intake
- Daily physical activity
- Better sleep habits
- Stress management strategies
Reduced hunger gives patients a valuable opportunity to build healthier eating patterns without feeling constantly restricted. Over time, these habits become easier to maintain.
As patients approach their target weight, treatment goals often shift toward maintenance and long-term stability. Some individuals continue using lower maintenance doses, while others transition to lifestyle-focused management alone.
Conclusion
Choosing Mounjaro in Dubai is not simply about rapid weight reduction. It is a structured metabolic health journey guided by science, consistency, and professional medical support. Each stage of treatment helps the body adapt gradually while improving blood sugar regulation, appetite control, and long-term wellness.
With proper supervision, realistic expectations, and healthy lifestyle integration, patients can achieve lasting metabolic improvements that support both physical and emotional well-being. At the conclusion of this journey, many individuals discover renewed confidence, improved energy, and a healthier relationship with food and their bodies. Tajmeels Clinic remains committed to supporting patients through every phase of safe and sustainable transformation.
health
Rhinoplasty for Men: Trends, Techniques, and Masculine Results
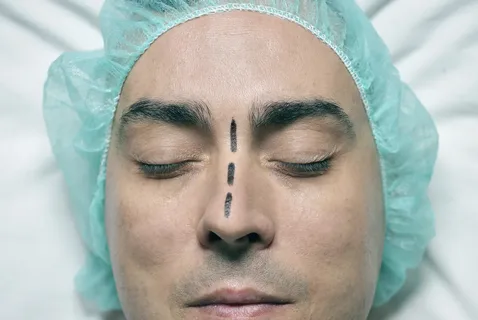
Cosmetic surgery is no longer limited to women, as more men are now seeking aesthetic treatments to improve facial appearance and confidence. One of the fastest-growing procedures among male patients is nose reshaping surgery because the nose has a major influence on overall facial balance. Rhinoplasty for Men in Islamabad has become increasingly popular among men who want natural-looking improvements while maintaining strong masculine features. Modern rhinoplasty for men focus on subtle enhancement, facial harmony, and functional improvement rather than dramatic cosmetic changes.
Growing Popularity of Rhinoplasty for Men
In recent years, social attitudes toward cosmetic procedures for men have changed significantly. More men now openly discuss appearance concerns and prioritize self-care, grooming, and facial aesthetics.
Rhinoplasty for Men has become a preferred option for men who want to improve the shape or structure of their nose without losing masculine characteristics. Many male patients seek correction for a crooked nose, prominent hump, wide bridge, or drooping tip while maintaining a natural appearance.
The increasing popularity of social media, professional networking, and digital communication has also influenced how men view their appearance. Many individuals want to feel more confident in photographs, videos, and face-to-face interactions.
Focus on Natural Masculine Features
One of the biggest trends in male rhinoplasty is the preference for natural and masculine results. Men generally do not want overly narrow or delicate noses because such features may appear unnatural on a masculine face.
Modern rhinoplasty techniques focus on preserving stronger nasal lines, defined bridges, and balanced proportions. The goal is to improve the appearance of the nose while ensuring it fits naturally with masculine facial features such as the jawline, forehead, and cheekbones.
This approach creates subtle enhancement rather than dramatic transformation, allowing patients to maintain their identity and facial character.
Reasons Men Choose Rhinoplasty
Men choose rhinoplasty for both cosmetic and functional reasons. Some individuals are unhappy with the appearance of their nose due to genetics, while others seek correction after injuries or breathing problems.
A prominent nasal hump is one of the most common concerns among male patients. Rhinoplasty can smooth the bridge while maintaining a masculine profile.
Many men also seek treatment for crooked noses caused by sports injuries, accidents, or trauma. Straightening the nose often improves both facial symmetry and nasal function.
Another common reason is refining the nasal tip. Men may want to correct a drooping or bulbous tip while preserving a natural and masculine appearance.
Functional Benefits for Male Patients
Functional improvement is a major reason many men consider rhinoplasty. Structural problems inside the nose can lead to breathing difficulties, snoring, or discomfort during exercise and physical activities.
Functional rhinoplasty helps improve airflow by correcting issues such as a deviated septum or nasal obstruction. Male patients often appreciate the ability to improve breathing while also enhancing the appearance of the nose.
Athletes and physically active individuals particularly value these functional improvements because better airflow can improve overall comfort and performance.
Influence of Modern Beauty
Beauty standards for men have evolved considerably over time. In the past, cosmetic surgery was often associated only with dramatic aesthetic changes, but today’s trends emphasize natural refinement and facial balance.
Men now seek treatments that help them look refreshed, confident, and well-groomed rather than surgically altered. Rhinoplasty fits this trend because subtle changes to the nose can greatly improve overall facial harmony.
Modern male beauty standards focus on confidence, symmetry, and proportion, which has increased interest in rhinoplasty procedures among younger and older men alike.
Techniques in Male Rhinoplasty
Modern rhinoplasty techniques have improved significantly, making procedures safer, more precise, and more customized for male patients.
Preservation rhinoplasty is one of the latest approaches used to maintain the natural structure of the nose while making subtle refinements. This technique helps create smooth and natural-looking results.
Structural rhinoplasty is also commonly used for male patients because it strengthens and supports the nasal framework while preserving masculine contours.
These advanced techniques allow surgeons to achieve balanced and natural results tailored specifically to male facial anatomy.
Personalized Treatment Planning
Every male patient has unique facial features and cosmetic goals. Personalized treatment planning is essential for creating successful rhinoplasty outcomes.
Surgeons carefully evaluate the patient’s facial proportions, nasal structure, skin thickness, and desired results before designing a treatment plan.
Men often prefer stronger nasal bridges and more defined profiles compared to female patients. The surgeon must understand these preferences to ensure the final result looks masculine and balanced.
Customized planning also helps preserve individuality and avoid results that appear unnatural or overcorrected.
Importance of Facial Harmony
The nose plays a central role in overall facial appearance. Even small irregularities can affect facial balance and draw attention away from other features.
Rhinoplasty improves facial harmony by refining the nose according to the patient’s natural proportions. Correcting asymmetry, reducing a hump, or refining the nasal tip can make the face appear more balanced and attractive.
For male patients, maintaining harmony between the nose and strong facial features is especially important. A successful rhinoplasty result enhances the face without making the surgery obvious.
Recovery and Healing Process
Modern rhinoplasty recovery is generally smoother than in the past because of advanced surgical methods and improved aftercare practices.
Male patients may experience temporary swelling and bruising after surgery, but these effects gradually improve over time. Most individuals return to routine activities within a few weeks.
The final shape of the nose continues to refine as healing progresses. Following post-operative instructions carefully is important for achieving the best possible results.
As recovery becomes more manageable, more men feel comfortable considering rhinoplasty for cosmetic or functional enhancement.
Psychological and Social Benefits
Many men who undergo rhinoplasty report increased confidence after improving the appearance of their nose. Since the nose is one of the most noticeable facial features, correcting long-term concerns can positively affect self-esteem.
Some individuals feel more confident during social interactions, business meetings, and photographs after surgery. Improved breathing function can also contribute to overall comfort and quality of life.
The psychological benefits of rhinoplasty often extend beyond physical appearance because patients feel more satisfied with their facial balance and presentation.
Choosing the Right Rhinoplasty Surgeon
Selecting an experienced rhinoplasty surgeon is one of the most important factors for achieving successful results. Male rhinoplasty requires an understanding of masculine facial anatomy and aesthetic preferences.
An experienced surgeon focuses on creating natural-looking improvements that maintain strong facial characteristics rather than producing overly refined or delicate features.
Proper consultation, realistic expectations, and personalized planning all contribute to successful rhinoplasty outcomes for male patients.
Final Thoughts
Male rhinoplasty has become increasingly popular because modern cosmetic trends focus on natural enhancement, facial harmony, and subtle refinement. Men today seek procedures that improve confidence while preserving masculine features and individuality. With advanced surgical techniques, customized treatment planning, and smoother recovery experiences, rhinoplasty offers effective cosmetic and functional benefits for male patients.
Care
Gallbladder Stones Treatment: Symptoms & Causes

If you have recently experienced a sudden, sharp pain in your upper abdomen or have been diagnosed with gallstones, you are likely looking for answers. Gallbladder stone, or cholelithiasis, are a common medical condition affecting millions worldwide. While they can remain “silent” for years, they can also lead to severe complications if left untreated.
In this guide, we will explore everything you need to know about gallbladder health and why consulting the best gallbladder surgeon is essential for effective, long-term relief.
Gallbladder Stone and How Stones Form
The gallbladder is a small, pear-shaped organ located on the right side of your abdomen, just beneath the liver. Its primary role is to act as a reservoir for bile—a digestive fluid produced by the liver that helps break down fats in the small intestine.
Gallstones form when there is an imbalance in the chemical composition of this bile. Most gallstones are made of cholesterol that has crystallized into hard deposits. Other stones, known as pigment stones, are made of bilirubin (a byproduct of red blood cell breakdown).
. A person can have one large stone, hundreds of tiny stones, or a combination of both.
Recognizing the Symptoms of Gallbladder Stone
Many individuals have gallstones and never know it. These are referred to as “silent stones” and generally do not require treatment. However, when a gallstone moves and blocks a bile duct, it triggers what is commonly known as a gallbladder attack (biliary colic).
Key symptoms include:
- Sudden, Intense Pain: Typically felt in the upper right quadrant of the abdomen or the center, just below the breastbone.
- Referred Pain: Pain that radiates to the right shoulder or between the shoulder blades.
- Digestive Issues: Frequent bloating, gas, and indigestion, especially after consuming high-fat meals.
- Nausea and Vomiting: Often accompanying the abdominal pain during an attack.
If you experience high fever, chills, or jaundice (yellowing of the skin and eyes), it could indicate a serious infection or a complete blockage of the common bile duct. In these cases, immediate medical attention is necessary.
Who is at Risk?
While anyone can develop gallstones, certain factors significantly increase your risk:
-
Dietary Habits: Diets high in fat and cholesterol and low in fiber are primary contributors.
-
Sedentary Lifestyle: A lack of physical activity can slow down the emptying of the gallbladder.
-
Gender and Age: Women are twice as likely as men to develop gallstones, often due to hormonal factors. The risk also increases for both genders after the age of 40.
-
Weight Fluctuations: Obesity is a major risk factor, but rapid weight loss can also cause the liver to secrete extra cholesterol, leading to stone formation.
Modern Surgical Solutions
Once gallstones become symptomatic, the standard medical recommendation is a Cholecystectomy—the surgical removal of the gallbladder. Because the gallbladder is an “extra” organ, your body can function perfectly without it; the liver will simply send bile directly to the small intestine.
Today, surgery is far more advanced than the traditional open procedures of the past. Modern techniques offered at specialized centers like Habilite Clinics prioritize quick recovery and minimal scarring.
1. Laparoscopic Cholecystectomy (Keyhole Surgery)
This is the gold standard for Gallbladder Stone removal. The surgeon makes 3 to 4 tiny incisions (each less than 1 cm) in the abdomen. A laparoscope (a thin tube with a camera) is inserted, allowing the surgeon to see the internal organs on a high-definition monitor.
- The Benefit: Most patients return home within 24 hours and can resume light activities within a week.
2. Robotic-Assisted Surgery
For complex cases or patients with previous abdominal surgeries, robotic assistance provides a higher degree of precision. The surgeon controls robotic arms that offer a 360-degree range of motion, which is even more flexible than a human wrist. This ensures that delicate structures like the bile duct are protected with the utmost care.
3. SILS (Single-Port Laparoscopic Surgery)
For patients concerned about the cosmetic outcome, SILS allows the surgeon to perform the entire procedure through a single tiny incision made inside the belly button. Once healed, the scar is virtually invisible.
Recovery and Life After Surgery
One of the most common questions patients ask is, “How will I eat after my gallbladder is gone?”
In the first few weeks following surgery, it is recommended to stick to low-fat meals to allow your digestive system to adjust. Over time, the body adapts, and most patients can return to a normal, healthy diet without any restrictions. Because the source of the pain (the stones) is removed, many find that their overall quality of life and digestion improve significantly.
Choosing the Right Specialist
At Habilite Clinics, we combine advanced technology with compassionate care to ensure our patients are back on their feet as quickly as possible. We specialize in minimally invasive techniques that reduce pain and help you return to your daily routine without the fear of another gallbladder attack.
Don’t ignore the warning signs. If you are struggling with abdominal pain or have been told you have stones, consult with the best gallbladder surgeon today to discuss a permanent solution.
-
Business3 years ago
Cybersecurity Consulting Company SequelNet Provides Critical IT Support Services to Medical Billing Firm, Medical Optimum
-
Business3 years ago
Team Communication Software Transforms Operations at Finance Innovate
-
Business3 years ago
Project Management Tool Transforms Long Island Business
-
Business3 years ago
How Alleviate Poverty Utilized IPPBX’s All-in-One Solution to Transform Lives in New York City
-
health3 years ago
Breast Cancer: The Imperative Role of Mammograms in Screening and Early Detection
-
Sports3 years ago
Unstoppable Collaboration: D.C.’s Citi Open and Silicon Valley Classic Unite to Propel Women’s Tennis to New Heights
-
Art /Entertainment3 years ago
Embracing Renewal: Sizdabedar Celebrations Unite Iranians in New York’s Eisenhower Park
-
Finance3 years ago
The Benefits of Starting a Side Hustle for Financial Freedom